Key Points
- Direct tensile loading of the biceps tendon is relatively minimal within the major powerlifting movements. Excessive stress, leading to biceps tendinopathy, is probably due to compression of the tendon against the surrounding soft tissue and bony structures.
- It is best to simply reduce stress along the involved tendon by manipulating training variables, allow the tendon reactivity to subside, and attempt to build specific tendon capacity through direct training when tolerance allows.
- During the bench, the primary point of interest is the bottom of the press. This position represents the most significant bottleneck of the lift due to the simultaneous compression and tensile strain experienced by the biceps tendon. Either avoid this posture entirely by employing bench variants that block bar descent (pin press, floor press, or board press) or use accommodating resistance to reduce loading in vulnerable positions.
- Save instability training for a later date. While evidence regarding the biceps role in shoulder stability is mixed, the added demands may place the biceps tendon under extra stress compared to more stable options.
- Swap out volume work performed on the bench to push-up and pressing variations, which do not constrain shoulder blade movement. This should help reduce any potential compressive stress experienced by the tendons due to altered scapulo-humeral dynamics.
- Pay attention to the upper arm position during all secondary and accessory lifts. Loading the shoulder in hyper-extended postures may provoke the sensitive tendon and limit tolerance to training globally.
- During the squat, the primary concern is the passive strain experienced along the anterior shoulder. Reduce humeral hyper-extension by switching to a false grip and drive the elbows farther under the bar. Move hands out to reduce shoulder external rotation.
- Build biceps tendon capacity by progressively loading the tissue. Begin using curl variations that place the shoulder in a passively flexed posture, with the goal to eventually perform the movement at greater angles of extension.
- Biceps tendon health is strongly correlated to rotator cuff function and integrity. Reduced rotator cuff capacity may increase intrinsic and extrinsic mechanisms of tendon degradation within the long head of the biceps tendon.
- Although no prospective evidence exists on this topic, it is probably wise to include exercises specific to the rotator cuff in programming to reduce compensatory strain experienced by the biceps within training.
When training or competing in the sport of powerlifting, significant stresses are frequently applied to the body in hopes of driving physiological adaptations. While injury rates in resistance training are fairly low when compared to other sports, they do occur.62 I wrote a previous article here on Stronger by Science to discuss a common lower extremity tendon pathology – patellar tendinopathy – and how to manage that condition without stepping away from training entirely. Now, I hope to turn that focus to a common complaint in the upper body: tendinopathy of the long head of the biceps. Anecdotally, this is a commonly assumed condition in the powerlifting community, particularly during training blocks with high frequency and/or volume of bench press and low bar back squats. I say “assumed” because there are MANY reasons why an athlete may experience anterior shoulder pain outside of biceps injuries.31 Although it almost goes without needing to be said, I will repeat my public service announcement:
This is not meant to be a replacement for a consult with a medical professional. If you are experiencing pain beyond what is deemed normal aches and pains associated with training, you should seek help for differential diagnosis and treatment.
My previous article outlined much of the current literature pertaining to tendon structure, function, adaptability, pathological states, and rehabilitation philosophy. Therefore, I will spend significantly less time outlining those concepts here, and I will instead explore additional training considerations. Important to note: Almost all of the data referenced in my previous article was gathered during studies pertaining to energy-storage tendons of the lower body. Additionally, I am unaware of any prospective studies evaluating the biceps tendon’s adaptability in response to deliberate loading. Confidence in these assertions should be adjusted accordingly.
What You’re Getting Into
This article is long. This is deliberate. The human body is exceedingly complex, and as such, a simple story is impossible to provide without watering down key aspects of the available information. Much of what is contained below is not directly applicable to individuals on a practical (or even a clinical) level; however, it does help fill in the gaps to help answer the “hows” and the “whys” behind the scenes. If that doesn’t interest you, feel free to skip around to the actionable sections (“Training: Alterations and Progressions” and “RC Training”).
Biceps Anatomy
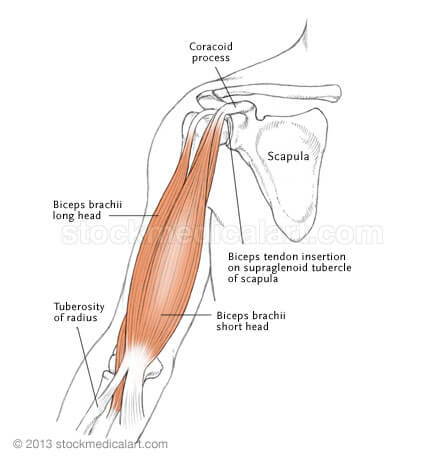
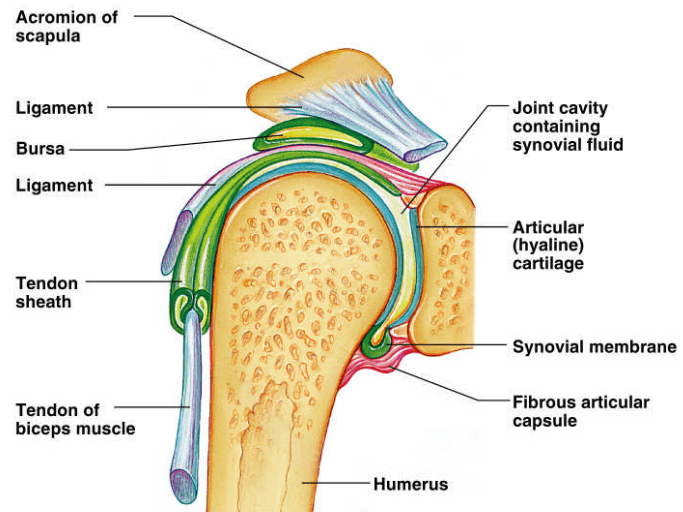
The biceps brachii is a two-headed muscle located in the anterior compartment of the upper arm. This muscle crosses both the shoulder and the elbow joints, since the long and short head each originate on the scapula and attach distally on the radial tuberosity.34 The long head of the biceps (LHB) tendon is considered intra-articular because it passes through the glenohumeral (GH) joint before exiting in the bicipital groove, a deep sulcus separating the greater and lesser tubercle of the humerus.23,34 From here, the extra-articular portion of the LHB tendon joins with the short head of the biceps tendon before complete conversion to muscle.66
Unlike many other tendons of the body, the biceps tendon differs because its line of traction does not match the line of pull of the adjoining musculature.53c This distinction occurs because the LHB tendon uses the head of the humerus as a pulley when applying tensional force. In order to prevent excessive compression at this site, an innate protective measure is put in place. A synovial sheath, arising from the synovium of the GH joint, surrounds the tendon to improve tolerance to the external stress and reduce frictional forces imparted on the soft tissue.52,53c,67
Biceps Function
The biceps act as a powerful forearm supinator and flexor of the elbow.34 However, the exact role that the LHB plays at the shoulder remains controversial. As an example, the LHB contribution to shoulder flexion has recently been called into question. A study conducted by Landin et al. demonstrated that as the shoulder flexes, the flexion moment provided by the biceps is essentially negligible after 30° due to the decreasing muscle length and reduced moment arm that occurs in this position.36 This finding is supported by EMG studies investigating the biceps, which control for potentially convoluting factors associated with the elbow joint. While using an external brace to passively lock the elbow in extended or flexed postures, it has been shown that outside of low-level activity observed within the first 30° of flexion and scaption, there is virtually no electrical activity of the biceps when performing flexion, scaption, external rotation, or internal rotation. This inactivity occurs regardless of the speed of movement or change in external loading (tested up to 5 lbs).38,72 Thus, in healthy adults, there is no clear consensus whether the biceps activity during shoulder movement is partly, mainly, or completely from the activation at the elbow joint.19 Important to note, these studies only investigated the shoulder from a neutral posture (0°) to a fully flexed posture. It remains to be seen if extending past neutral would alter this relationship since the LHB tendon length and moment arm in this position could lead to an enhanced role.
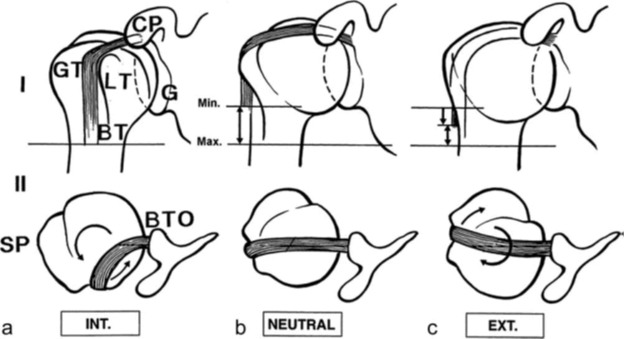
It is commonly assumed that the LHB serves as both an active and passive humeral head depressor and stabilizer of the GH joint.23 The stabilization provided by the LHB has been postulated to restrain total rotation of the shoulder joint and reduce intra-articular movement of the humerus. During positions such as the late cocking phase of throwing, the biceps’ value in preserving dynamic anatomical integrity is thought to be particularly important.20,32,59 Anterior shoulder stability is of significant concern in this position because 95% of all dislocations occur in this direction.16 As the shoulder approaches the “high five” position (90° abduction with 90° external rotation), the joint is especially vulnerable because the rotator cuff becomes less effective at preventing anterior translation of the humeral head due to reduced moment arm lengths.1b Fortunately, while the RC becomes progressively inefficient as the arm is abducted and rotated, the biceps role in stabilization is enhanced.32,46 Due to the roll and glide of the humeral head during shoulder movement, the relationship of the biceps tendon with its attachment site on the scapula changes based on arm position (see image below). When the arm is below 45° of elevation, the tendon alignment encourages GH rotation and, when above 45°, the line of pull restricts motion.20
Figure 3 from Eshuis et al.20
Demonstrating the facilitatory role when under 45°
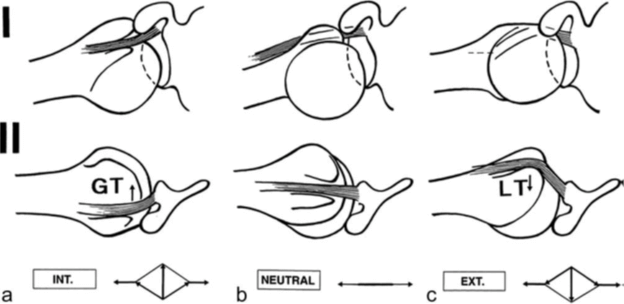
Figure 4 from Eshuis et al.20
Demonstrating the restrictive role when over 45°.
CP= Coracoid Process, GT= Greater tubercle, LT= lesser tubercle, BT= biceps tendon, G=glenoid, BTO= biceps tendon origin, SP= scapular plane
This theoretical model of function is corroborated by cadaveric studies. When removing or applying external tension to the biceps musculature at low angles of arm elevation, Kuhn et al. noted no difference in total GH range of motion.32 But, when applying tension when the arm was positioned in an abducted and externally rotated posture, the group found significant reduction in total motion. Additionally, this suppressive ability also seemingly fits with EMG data. Electrical activity of the biceps has been shown to increase significantly at greater angles of elevation and external rotation. Although there are concerns with this argument (to be discussed later), these data provide evidence to support the idea of a position-specific role for the LHB.46
Tendinopathy
As previously mentioned, pathological changes in tendons are due to a mismatch in loading. The term “overuse” provides an overly simplified portrayal of the condition. Instead, the process is more aptly characterized as a fluctuating ratio. When the applied loads (magnitude/frequency/rate) exceed our body’s ability to respond, the result is pathology.
The mechanism of injury and the subsequent rehabilitative intervention is a straightforward process with the patellar tendon. Pathology occurs when the internal loading of the tendon (such as tensile stress during squatting) exceeds the adaptive capacity of the tissue. The intervention is simply a modification of the dosage of the activity. For the squat, variables are manipulated to allow for sufficient loading of the involved tissues while the rate of progression is (auto-)regulated to afford adequate recovery.
The long head of the biceps tendon presents a different challenge entirely because the main movements within powerlifting evoke fairly low-level activation of the biceps musculature.55,64,68 Without the obvious tensile stress, it is less apparent why biceps tendons enter a pathological state during intense blocks of training. The likely culprit for the degenerative progression is a previously unmentioned consideration: compression.
Compression
While compressive stress is thought to play a minimal role in the pathological progression of patellar tendinopathy, it is considered a key contributor to LHB tendon injury.9,10,13,18,37,73 Due to the anatomical orientation of the biceps tendon in relation to the humeral head, there are frequent compressive forces imparted upon the soft tissue. The level of stress experienced is directly influenced by the position of the shoulder. Anterior translation or superior migration of the bony structure will strain the surrounding soft tissue. This intra-articular movement, and subsequent compression, is commonly seen when performing humeral extension beyond neutral (behind the body) or when lifting the arm above certain angles.
To fully appreciate this concept, an understanding of the influence mechanical stress has on tendon properties is required. Tenocytes (tendon cells) are capable of detecting and converting mechanical stimuli into biochemical responses, a process termed mechanotransduction.18,29 This link is imperative for the survival and adaptation of biological organisms. Tenocytes respond to applied stressors in a specific manner in order to help the tissue tolerate imposed demands.13b,18 However, this process can falter if the rate, intensity, frequency, and/or volume of stress exceeds the tendon’s adaptive capacity.28,44b When studied in isolation, compressive loading actually has minimal effects on tendon properties. But, when combined with tensile loading, the resulting effects have been described as “especially damaging to the tendon.”18
Compression to the LHB tendon arises externally from two main sources: the coracoacromial arch and the bicipital groove.
One of the most discussed sources of external stress to the LHB tendon is the mechanical compression of the tissue against the acromion process and the coracoacromial ligament during shoulder flexion.9,10,14,73 This phenomenon is known as subacromial impingement syndrome (SAIS) and is defined as “compression or abrasion of the cuff tendons or tendon of the long head of the biceps brachii beneath any aspect of the coracoacromial arch.”40 Impingement is proposed to occur during shoulder flexion, abduction, or horizontal adduction above 90° and is increased when the arm is internally rotated. Structural factors (anatomical variations of the humeral head, acromion, and/or scapula) and functional factors (RC strength and integrity, joint capsule pliability, muscular tightness, scapular neuromuscular control) have both been correlated to the total distance between the superior aspect of the humeral head and the acromion process. Therefore, these qualities and traits have long been assumed to contribute to various shoulder conditions.
This concept is not without controversy as it has been shown that soft tissue impingement occurs naturally in all shoulders during flexion and abduction at angles as low as 30°.7b Thus, it is reasonable to question if SAIS has a causative role in the development of tendon pathology. That said, even if SAIS does not drive the initial tendon damage, it is a source of compression and may have significant implications for tendinopathy provocation or progression.
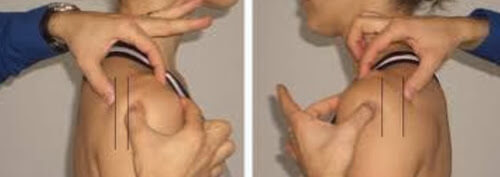
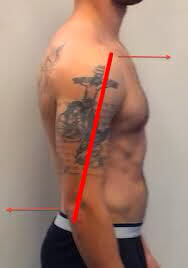
Finally, beyond humeral hyperextension and subacromial impingement, the humerus may also interact with the LHB tendon in other consequential ways. The first occurs when there is isolated movement of the humerus on a stationary scapula. Dr. Shirely Sahrmann originally introduced the concept of humeral anterior glide syndrome, which has later been represented in formal literature as humeral head anterior glide posture (HHAGP).26,57 The image below demonstrates HHAGP with more than one third of the humeral head protruding from the anterior acromion- positioning the humeral head more anteriorly than the distal humerus (aka the proximal and distal ends are not aligned in the same vertical plane).26
The second way in which this compression manifests is through changes in relative structural alignment. If the scapula is anteriorly tilted (pitched forward), the humerus is relatively placed into an extended position despite the general appearance of neutrality. Thus, the proximal biceps tendon is subjected to similar levels of stress as it would be during extension beyond neutral.
An important caveat is the difference between static and dynamic postures and their respective relationships with pain and pathology. When it comes to static positioning of the thoracic spine and shoulder girdle, systematic reviews reveal no significant evidence to indicate static posture affects pain.3 As Paul Ingraham wrote in his excellent article, “the idea of ‘poor posture’ is mostly much ado about nothing — a problem in theory, but usually not much of one in practice.”
However, dynamic postural alignment is a different consideration all together. Postural positioning can have an impact on the ability to generate force as well as the distribution of stress among the working tissues.41 As the constraints of the intended task become more specific (increase in load lifted and/or repetitions performed), there are fewer options for safe and effective performance. Altered alignment of the shoulder joint (leading to increased compression) may be well-tolerated when performing lower intensity lifts, but may have ramifications when combined with high-intensity tensile stresses. Although, scapular and/or humeral posture has not been studied within this context so any arguments to this effect are purely speculative.
Training: Alterations and Progressions
As alluded to earlier, even though the tensile load on the proximal biceps tendon during primary lifts is relatively low, it is often combined with compressive forces. This stress pattern makes the major movements a poor choice for rehabilitation. Instead, it is best to modify the lifts to reduce specific loading below the provocative threshold in a manner which is customized to suit the needs and goals of the individual. While prepping for an upcoming meet, the squat, bench, and deadlift should obviously be kept as close to performance standards as tolerance allows. In such instances, it is better to manipulate loading elsewhere within the program. Alternatively, if there is no immediate need to perform at peak levels, there is much more room for flexibility in the big three. The nuts and bolts of individualization are left to the individual.
Bench
Historically, the biceps tendon has been considered a stabilizer and an antagonist during the bench press.64 When examined under more formal conditions, this notion loses merit. Several studies have looked at EMG values of the biceps during the bench press, and it has been determined that absolute electrical activity is low compared to the primary agonists across a broad spectrum of parameters – observed during both maximum effort lifts and higher volume sets performed to failure.55,68 This relative inactivity supports the argument that stress on the LHBT during benching primarily derives from an external compressive force rather than direct tensional loading.
Mechanics and Variant Selection
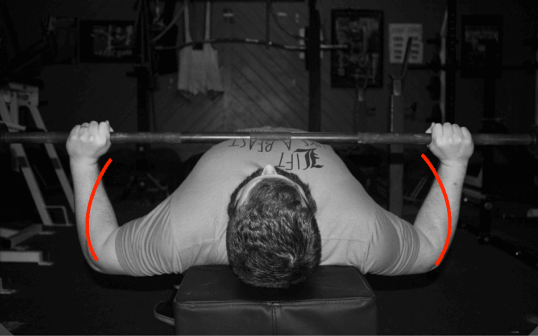
Limiting total range of motion, or load at the bottom of the movement, is the most important factor when managing biceps tendon stress within the bench press. What I want to draw focus to in the above image is the angle between the elbow and the top of the shoulder. This position represents the most significant stress imparted on the LHB tendon during the bench. The angle achieved at the bottom of the press is influenced by several factors (chest circumference, grip width, amount of elbow tuck) so the resultant strain will vary between individuals. Load in the bottom of the bench press can be changed in a number of ways and simply modifying one of the above components may be sufficient to limit humeral extension enough to grant the ability to press pain-free. Trying different grips and arm angles will help to determine if a small tweak is all that is necessary. If minor changes don’t eliminate the pain, more drastic options may be required. An almost foolproof method to prevent a lifter from obtaining this compressive orientation entirely is by switching to the floor press or pin press (I say almost foolproof because some individuals put themselves in the same relative shoulder posture by excessively arching their thoracic spines during these movements). Or, if attempting to keep the eccentric-concentric coupling of the movement intact, a board press can function as a great alternative while still eliminating the irritating range of motion. My recommendation would be to experiment with a preferred variation and find the range and intensity that allow for pain-free pressing. This change is often all that is necessary to reduce loading below a problematic threshold and allow for continued training. If not, there are other variables which can be manipulated to further influence impact on the biceps tendon.
Loading
When the standard press is performed, how the range of motion is loaded should be examined. Since compression and tensile stress is the theorized mechanism of provocation, the bottom of the bench represents a significant bottleneck to the weight selected; therefore, the inclusion of accommodating resistance is extremely valuable. If available, bands or chains are recommended to maximize efficiency of training in these early stages. They both serve to reduce tensile strain at vulnerable positions while still providing sufficient intensity throughout the remainder of the press.
Velocity
As outlined in my previous article, tendons display both time-dependent and time-independent characteristics due to their viscoelastic properties. High speed contractions demonstrate significantly different musculotendinous dynamics (and stress) when compared to slower contractions.18c,54c Thus, the rate at which stress is applied has an impact on the tendon.18c,45 Deliberately slow cadences are used in rehabilitation to minimize adverse responses to loading. Accordingly, adopting an intentionally slow tempo (2-4 second concentrically and eccentrically) should allow for greater total intensities to be tolerated when training for performance as well.
Stability
Due to the LHB tendon’s proposed function as a glenohumeral stabilizer, one would assume a clear association would be observed between task stability demands and biceps activity. That is not the case, as current data regarding this notion is equivocal.22,51,53,55,56 Interestingly, the divergent outcomes seem to stem from the location of instability. Studies that change the inherent stability of the base of support (lying on a bench versus a stability ball) routinely find no differences in biceps EMG activity.51,55 Conversely, studies that manipulate distal stability (using dumbbells versus barbell versus a Smith machine) often show an inverse relationship between stability and biceps contribution.22,56 But, to muddy the water further, the magnitude of this finding is small and inconsistent, with conflicting reports on its existence.53 Practically, however, this may indicate that the use of less stable training modalities may place greater demands on the biceps than more stable alternatives. Thus, it may be wise to limit total volume performed with dumbbells (or other loading strategies like bamboo bars, which create distal instability) during the initial phases of rehab. That said, there are no hard-and-fast rules when navigating this condition. Values regarding the magnitude of stress the biceps experience within these studies are not placed into any meaningful context. This makes comparing the impact instability has versus joint angles or total range of motion difficult. If training with dumbbells is desired, simply modify the range and velocity as outlined above to determine tolerance.
Scapular Mobility
Scapular kinematics are undeniably important to shoulder function. As has been discussed throughout this article, the position of the humeral head within the glenoid (the lateral aspect of the scapula) has substantial consequences for the surrounding soft tissues during dynamic tasks. Any isolated movement of the articulating surface would change the relative location of the humerus, impacting nearby structures such as the LHB tendon. To understand how this can be meaningfully influenced, a solid understanding of normal scapulothoracic mechanics must be established.
The scapula is only minimally supported by geometric and anatomical constraints, instead relying heavily on the 17 musculotendinous attachments for static and dynamic positioning.48 This design is important for the functionality of the shoulder complex. Lack of structural rigidity affords extreme mobility of the scapula, an essential feature to ensure glenohumeral orientation and length-tension relationships of the acting musculature are preserved as the arm elevates.
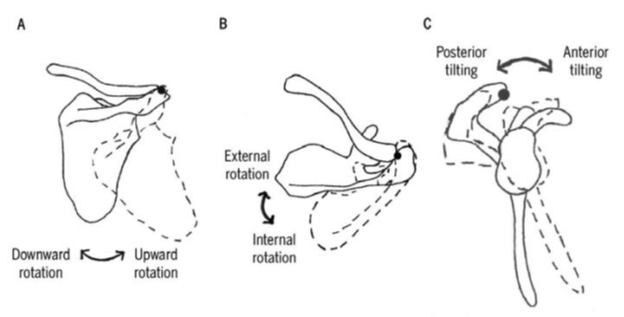
Figure from Ludewig et al.41
Along with elevation/depression and adduction/abduction, the scapula rotates in three dimensions (see image above). Recent evidence indicates there is an average of a 2.3:1 ratio of humeral to scapular movement, meaning for every 2.3° of humeral elevation, there is 1° of scapular upward rotation.6 Although the exact ratio of scapulohumeral movement may vary depending on external demands and speed of movement, the consistent finding is that during humeral elevation, the scapula tilts posteriorly, upwardly rotates, and externally rotates.6,48 Deviations from this norm are often referred to as “scapular dyskinesis,” and this condition has been implicated in several pathological conditions of the shoulder.41 Pertaining to this discussion, a major theory regarding irregular scapulohumeral rhythm is that it may compromise the LHB tendon and rotator cuff tissues by contributing to SAIS.40
Mini tangent: Hold on before you assess your scapular kinematics and self-diagnose yourself with dyskinesis. This remains a highly contentious topic within the world of physical therapy. A growing opinion is that what is often labeled pathological may simply be normal movement variation.48 Even if the scapular dynamics represent a deviation from an individual’s normal pattern, an emerging theory is that the changes may be natural compensatory measures adopted to offload the sensitized structures.
The question becomes “what does this have to do with the bench press?” While benching, lifters consciously suppress natural scapular rotation by actively retracting their shoulder blades throughout the movement. This is compounded by the fact that a physical restraint (the bench itself) is further limiting the normal shoulder blade movement necessary to reduce compressive loading of the LHB tendon and RC tendons. While this level of stress is obviously endurable for the vast majority of individuals, the vast majority of the time, it may be problematic for those who are currently dealing with loading intolerance. Thus, loaded push-ups offer a viable solution to assist within this particular context. By removing the physical constraints and intentionally moving the shoulder blades through their full range of motion, the compressive stress imparted upon the LHB tendon is potentially reduced. Removing the barbell bench entirely from programming is excessive and probably unnecessary. Under most circumstances, especially with the inclusion of the adjustments noted above, some level of pressing is probably tolerable and beneficial to keep in training. But, for the accessory and volume work, swapping out standard bench press variations for push-ups may pay dividends early in the rehab process.
Side note: If you’re a member of USAPL, my friend and colleague Michael Soya wrote an article on benching with biceps tendinopathy last year for their magazine. It’s worth looking into if you want more perspective on the topic.
Squat
There is no major active demand placed upon the shoulder within the squat. The stress incurred is attributable to the positioning of the shoulder during the movement. Lifters are often (rightfully) advised to adopt a narrow hand position in attempts to generate tension and create a stable shelf for the bar to rest. Greg has written about this in the past, with the advice to place hands “as close as you can comfortably get them.” Unfortunately, the part regarding “comfortably” is often glossed over with individuals assuming positions that put their shoulders under unnecessary duress. Those experiencing chronic shoulder discomfort would do well to reassess their current setup.
As discussed at length, provocative positions for the anterior aspect of the shoulder (including the LHB tendon) include combinations of humeral extension, abduction, and external rotation. The rack position often combines all three elements. While it may seem as though this posture would be intolerable when dealing with biceps injuries, there is room for optimism. Upon examination of Massimini et al.’s data regarding humeral head movement, an interesting finding emerged. As the shoulder was externally rotated in an abducted position, the group found no noticeable changes in the anterior position of the bony anatomy through the majority of the motion. But, as end-range rotation was approached, there was a significant forward shift of the proximal humerus.47 This means the potentially instigating humeral translation appears to be contingent upon the available range of motion of the individual. Therefore, there is probably a wide range of positions the shoulder can safely obtain during the back squat without inducing any negative consequences; although, if the shoulder is placed in end range rotation, the squat may prove problematic.
Two simple adjustments can significantly reduce the likelihood of anterior shoulder strain.
First, to reduce positional stress within the squat of choice, move from a thumb-under grip to a false grip. This change allows the elbows to be driven farther under the bar – instantly reducing humeral extension without compromising wrist neutrality (as can be visualized above).
Second, if still experiencing discomfort in the rack position, I recommend checking hand placement. To put it simply, widen the grip. Moving grip out allows a lifter to obtain the same relative hand position with less external rotation, thus reducing any tensile and/or compressive loading associated with said posture. While this wider placement may lead to the perception of less upper back tension, this can mostly be compensated for by actively contracting the lats. Greg’s cue of “scratch your rib cage with your elbows” works well here.
Finally, if unable to find a position that allows for pain-free training, there are still alternatives that should prevent eliminating the barbell all together. Unless gearing up for a meet, temporarily incorporating a different squat variation is a worthwhile consideration. A front squat or safety bar squat will eliminate the problematic posture entirely. Thus, approximately the same stimulus can be achieved with significantly reduced strain along the anterior shoulder.
Secondary and Accessory Lifts
When dealing with biceps tendinopathy, there are two main considerations pertaining to lifts outside of the big three: exercise selection and exercise form.
When it comes to exercise selection, the popular trend is to paint black and white pictures of movements as being “safe” or “dangerous.” This sensationalist notion is unwarranted. Exercises are merely methods of applying stress to the body in a concerted effort to drive adaptations. An individual movement is not at fault for an injury. That blame belongs to the poor program design and application of exercises that are inappropriate (either in intensity, volume, rate, or range of motion) for the current capacity of the lifter.
The responsibility falls on the person designing the program to understand the current tissue tolerance and the ways in which specific exercise performance will affect that tissue. As previously stated, it may be beneficial to minimize the inclusion of exercises that alter normal scapular dynamics. When able, switch supine exercises to push-up and press variations, which do not constrain shoulder blade upward rotation. Additionally, when attempting to reduce total load along the LHB tendon, it is best to limit exposure to high levels of compressive stress early in the rehab process. Thus, movements that put the humerus in hyperextended postures (dips) should probably be temporarily avoided.
There are many more lifts that can be subtly altered to avoid excessive strain of the biceps. The common element is restricting range to keep the humerus in front of the body. Most importantly, this sentiment applies to pulling variations. When performing rows, it’s common to see the scapula remain protracted and anteriorly tilted throughout the movement, while the humerus is driven back beyond the plane of the torso (See image below for an example).
This posture combines high tensile loads (due to the biceps role in elbow flexion) with potential compression proximally (due to the scapular and humeral head orientation). The simple solution is to deliberately retract the shoulder blade in conjunction with the upper arm movement. Anecdotally, I find that if the lifter focuses their attention on this process and prevents an anterior tilt of the scapula, the extension range is naturally restricted from venturing far beyond the trunk.
Direct Biceps Training
Altering external stress is the most important step to reducing total tendon load below the critical threshold. While program adjustments are often enough to stave off symptom provocation, it is probably wise to include exercises that attempt to enhance the capacity of the involved tendon.12 By evoking physiological adaptations of the LHB tendon, and subsequently improving stress tolerance, resiliency may be improved moving forward. Again, the specific changes of the LHB tendon in response to loading are not thoroughly investigated at this point in time. Therefore, I will default to making recommendations based on the more robust evidence observed from tendons in the lower body. Although I am unaware of any major physiological rationale for why the resulting adaptations would substantially differ, this extrapolation does leave open the possibility that these recommendations are inaccurate or incomplete. Keep an open mind and understand that these guidelines are subject to change.
Exercise Selection and Progression
Begin conditioning the involved biceps tendon by using a curl variation that does not place the tissue under compressive loading.13 This means that putting the shoulder in a passively flexed posture (preacher curl, supine curls on an incline bench) is probably a good starting place. Over time, as tolerance allows, gradually progress the shoulder angle into greater humeral extension with the eventual goal of performing incline curls.
Intensity
Unlike muscle tissue, which responds to a wide variety of stimuli, tendons require more specific loading parameters.5b,50b Tendons often fail to display evidence of mechanical, material, or morphological adaptations when loaded below 70% 1RM, leading to the postulation that greater stress levels are necessary to induce the cell deformation required to kickstart the adaptive cascade.5b Therefore, it is most likely best to choose a weight no lower than your 10-15 rep max.
Performance
While I doubt many readers are performing dynamic effort days with their biceps work, tempo should still be a concern. As discussed, tendons are sensitive to their rate of loading. Slow tempos (2-4 seconds) should be encouraged during the eccentric phase of the lift to reduce absolute tendon strain.18c,45
Frequency
Beneficial adaptations in response to loading require net protein synthesis. Following resistance training, enzymatic activity stimulates both protein synthesis and degradation in collagen fibers. Initially, there is a net protein loss, with a net gain not observed until approximately 36 hours after exercise.44b Therefore, it is believed that for positive adaptations to be observed, a certain restitution period is beneficial. Provide at least 36-48 hours between loading sessions to assist the recovery process.
Rehab Duration
Tendon material properties are relatively unchanged until after approximately 8-12 weeks of specific load application. Additionally, morphological adaptations likely take much longer (currently, no definite time-course for adaptation has been agreed upon, but consistent findings appear after years of training).5b,71b This implies that an intentional inclusion of specific rehabilitative efforts should be maintained for at least three months following injury, if not longer.
Why might this be occurring? Is there anything to do to help reduce chances of injury or reinjury?
Other Potential Mechanisms of Biceps Tendon Injury
As alluded to earlier, the long head of the biceps tendon has been proposed to be a secondary stabilizer of the humeral head within the glenoid fossa during dynamic shoulder functions.73 The bulk of the evidence that supports this notion comes from studies performed on cadavers, with results indicating the LHB depresses the humeral head and adds compression to reduce articular motion.19 However, there is a strong contention that data obtained through cadaveric testing fails to accurately represent shoulder function within living subjects, as 1) the level of electrical stimulation and/or external tension applied to the biceps may exceed physiological norms and 2) there is a failure to “recreate the myriad of factors that act in synergy to provide glenohumeral stability in vivo.”19
Fortunately, this hypothesis was recently put to the test by Giphart et al. in living humans.24 The research group used video fluoroscopy to determine the intra-articular movement of the GH joint in patients who had undergone biceps tenodesis procedures. This surgical intervention detaches the LHB from the superior labrum and anchors it to the shaft of the humerus, thus eliminating any compressive force it may apply to the head of the humerus. While performing abduction, lifting (flexion with the forearm supinated), and simulated throwing tasks, the subjects were monitored. Their results were contrasted against their opposite, uninjured shoulders. The majority of measurements did not meet statistical significance, with the exceptions being the tenodesed shoulders were, on average, 0.7 mm and 0.9 mm more anterior during abduction and throwing respectively. Notably, these discrepancies actually represented a reduction in humeral motion rather than the commonly proposed instability, as the anterior position placed the shoulders more centered than their counterparts. The small differences observed are unlikely to be of clinical significance, and even if they are, the translations observed in tenodesed shoulders were LESS than are seen in normal shoulders. Therefore, the researchers concluded “structures of the shoulder, such as the surrounding musculature, are producing significantly higher forces at the glenohumeral joint in vivo, such that the contribution of the biceps provides a minimal secondary stabilizing role when these other stabilizing structures are intact.”24
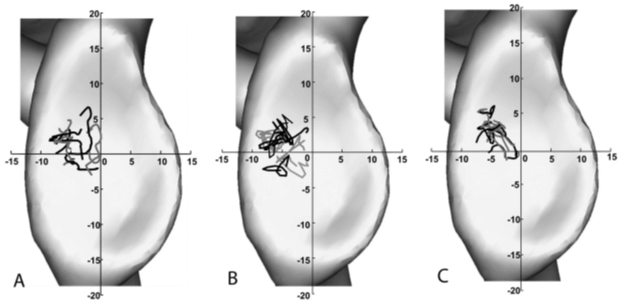
Path of glenohumeral motion graphed for all patients, with gray lines representing the tenodesed shoulders and black lines representing the healthy contralateral shoulders: (A) abduction, (B) simulated late cocking phase of a throw, and (C) simulated lifting task. The glenoid image is scaled to represent the approximate average glenoid size and is provided for visual reference only.
Rotator Cuff: Cause, Consequence, or Spurious Correlation?
So, based on the presented evidence, it may appear that the biceps’ role in intra-articular stability is minimal at best and our efforts are better allocated to addressing the mechanical loading of the tendon within training. Not so fast. The final caveat of the quotation from Giphart is important – “when these other stabilizing structures are intact.” The story changes drastically if there is a loss of integrity or capacity of the rotator cuff. It is currently speculated that only 5% of all LHB tendinopathies are of primary origin, with the remaining 95% hypothesized to be secondary to other shoulder disorders (particularly rotator cuff pathologies).53b
The relationship between lesions of the rotator cuff and the biceps tendon have been studied extensively. Redondo-Alonso et al. conducted a systematic review to assess the literature pertaining specifically to the association of pathologies between the supraspinatus tendon and the long head of the biceps tendon.54 Within these studies, there was a clear association of lesions in the aforementioned tendons, with concomitant pathologies ranging from 22% to 78.5%. Additionally, studies that did not limit their findings to one specific rotator cuff tendon have found consistently higher correlations. For example, Dr. Chih-Hwa Chen and his colleagues have published two papers that have found associated rates between 75% to 97%, and they determined a positive correlation between RC tear size, RC tear chronicity, and number of RC tendons torn with the likelihood of biceps tendon damage.9,10 However, each study analyzed within the systematic review and those conducted by Chen were assessing cohorts that (almost) all had known rotator cuff tendon pathologies. So, while this data strongly indicates there is a correlation between the conditions, it does not aid in answering the question of causality.
To address this question, a closer look at prevalence data is required. Unfortunately, I was not able to find any epidemiological rates pertaining to isolated biceps pathologies, only allusions to the condition being rare outside of specific contexts (primarily observed in throwing athletes). While still unable to answer the question of “why,” Chang et al. provide interesting data that can be used to move this conversation forward.8 The group quantitatively assessed 1,389 shoulders using ultrasound imaging and, within that sample, found 160 full tears of the supraspinatus tendon and 17 biceps tendon tears. The researchers were concerned with the predictive ability of biceps tears to determine the presence of supraspinatus tears. A risk ratio of 8.1 was determined for this relationship; in other words, an individual with a biceps tendon tear was 8.1 times more likely to have a supraspinatus tear compared to an individual without a biceps tendon tear. What I’d like to call attention to is that Chang et al. missed an obvious correlation within this data. If the relationship is reversed (i.e. if we assess the risk of biceps tears in the presence of supraspinatus tears), the results create a striking impression. 15 of the 17 torn biceps tendons were in the group of 160 who additionally had supraspinatus pathologies. Thus, of the remaining 1,229 participants without supraspinatus abnormalities, only 2 had biceps pathologies. This means the risk ratio is 55.7 according to their findings. There is ample reason to believe that the patients analyzed in this data are not reflective of the general population or the true relative risk of biceps pathologies after rotator cuff injuries. However, this observation does serve to raise intrigue into the potentially sequential nature of these conditions. How could a pre-existing rotator cuff tear increase risk of a future bicep injury? And if this succession does occur, what can we do to impede this possible progression?
Rotator Cuff Anatomy and Function
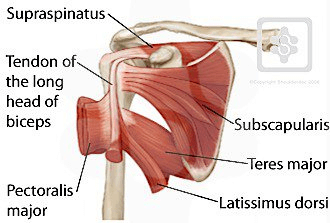
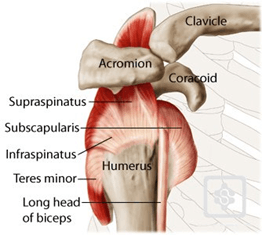
To adequately unpack this association, a complete understanding of the rotator cuff’s role is necessary. The rotator cuff is a group of four tendons (supraspinatus, infraspinatus, subscapularis, and teres minor) that each have distinct musculotendinous actions when assessed in isolation. The grouping is made because the tendons fuse to form a continuous structure that acts as a functional unit to stabilize the shoulder joint through compression of the humeral head into the glenoid cavity.28,50
Poor rotator cuff capacity is proposed to alter glenohumeral kinematics and lead to changes in stress distribution within the surrounding soft tissues.63 To reiterate, alterations in humeral head dynamics are a commonly offered mechanism for biceps tendon injury, often theorized that resulting glenohumeral instability exposes the biceps tendon to greater levels of stress.9,10,15,73 Traditionally, it has been argued that insufficient RC capacity leads to excessive superior migration of the humeral head during shoulder demands, inducing compression of soft tissue against the coracoacromial arch. Consistent with many concepts introduced within this article, this simple narrative has lost support as recent advancement of imaging technology suggests this instability may not occur at all in the presence of RC tears.50 However, regardless of the eventual realizations, current evidence suggests there are alterations in tissue demands following rotator cuff pathology that require accommodation, and the biceps tendon is (probably) partly responsible for filling the void.
Warning: The next section takes a deeper look into the relationship between the rotator cuff and the long head of the biceps tendon. While I obviously feel this adds valuable context to the discussion, it is by no means necessary from a pragmatic standpoint. For my fellow musculoskeletal geeks or practicing clinicians, read on. For those who just want the practical takeaways, skip to the “so what” section.
Compromised rotator cuff structure and strength has been demonstrated to influence the biceps tendon in multiple ways, and this impact can be broadly categorized into two main groups: intrinsic mechanisms and extrinsic mechanisms.
An intrinsic mechanism of pathology refers to change in the tendon physiology stemming from natural processes of aging and/or demands on the tendon cells that exceed their remodelling capacity.44,60 Therefore, intrinsic factors of degeneration can be considered as internal processes of the tendon itself and serve to explain the direct relationship observed between age and tendon pathology.69 An extrinsic mechanism of pathology refers to degeneration that spawns from an application of stress from outside of the tendon. This can be thought of as stress imparted on the biceps tendon from an external source, which may contribute to the deterioration of the structural integrity.43,60
Intrinsic Factors
The most obvious source of internal stress on the LHB tendon comes from loading during various upper extremity exercises. Health of the rotator cuff may intimately influence the magnitude of stress experienced during training, as it is often argued that the LHB tendon bears an increased burden in the presence of RC dysfunction.5,30,33,58 Kido et al. provide indirect evidence in favor of this contention when they measured EMG activity during shoulder flexion in a group with known rotator cuff tears.30 Increased EMG levels of the biceps were found when comparing between subjects’ involved (known RC tear), and uninvolved (no RC tear) arms. Additionally, a significant increase in biceps activity within RC-compromised shoulders was observed when adding weight (1kg) compared to an unloaded condition. This increase indicates that the compensatory demands placed upon the LHB tendon may be magnified during resistance training efforts. This study does not allow for claims to be made regarding less severe conditions (RC tendinopathy as opposed to tear), does not have additional conditions to determine if EMG levels would rise linearly with increasing external demands, and does not provide any direct measurement of humeral positioning between conditions; however, it does serve as a proof of concept for the original hypothesis.30
More recent indirect support of increased loading is provided through Michael Kurdziel’s work.33 While examining structural and mechanical differences between LHB tendons in individuals with and without RC pathologies, his team discovered significant discrepancies at each level of organization. Particularly, several key adaptations were observed that suggest excessive loading of the biceps in this specific context. Biceps tendons from RC-deficient shoulders displayed significantly reduced collagen fiber alignment compared to fibers from within RC-intact shoulders. Furthermore, when assessing stress/strain characteristics, stress prior to tendon failure did not differ between groups, but the amount of elongation did (in favor of the RC deficient tissues). These findings fit with previously discussed adaptations observed in pathological tendons. Thus, even without the formal label of tendinopathy provided, the data from Kurdziel’s study indicates precisely what we’d speculate to occur if the biceps were placed under chronically excessive stress: similar absolute loading capacity with decreased tendon stiffness. Therefore, there is at least preliminary support for the notion that rotator cuff pathology results in amplified internal loading of the biceps tendon.
Aside from the biomechanical changes noted above, increased loading of the biceps tendon leads to other intrinsic deviations that deserve brief acknowledgement. Previous data have correlated the presence and extent of rotator cuff damage to genetic, hormonal, and vascular changes within the proximal biceps tendon.33,35 The down-regulation of several genes responsible for protein synthesis may lead to reduced adaptive capacity of the tendon in response to loading, and in turn, propagate the pathological process.33 Additionally, vascular ingrowth into the degenerative tendon is thought to be a natural part of the repair and remodelling process following microtrauma. Unfortunately, this process can lead to further reduction of mechanical stability and contribute to an unwanted positive feedback loop of pain and dysfunction.35
Extrinsic Factors
The most championed theory pertaining to external stress upon the biceps tendon is through direct compression against the coracoacromial arch. As discussed above, the importance of SAIS is widely debated. There are strong arguments in opposition to the phenomenon’s significance, with some even going so far as to call for the abandonment of the term entirely due to its failure to adequately explain the clinical manifestations observed.28,42 However, if we accept the premise that chronically compromised RC capacity may induce kinematic alterations, and that the combination of compressive and tensile loading is a contributing factor to degenerative tendon changes, it seems logical that the described scenario would contribute to LHB tendinopathy in a meaningful way.13,15,18 But, due to the paucity of high-quality evidence in favor of this specifically altered joint movement, the premise continues to require a suspension of disbelief. Hopefully, advancing technology will grant clearer answers to this contention in upcoming years.
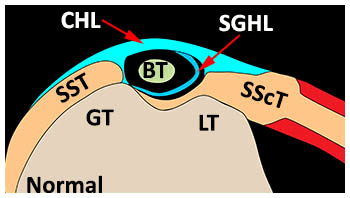
A more well-regarded way in which the health of the rotator cuff is inextricably linked to biceps tendon integrity is through the mechanical contribution several cuff tendons provide to the biceps pulley. Before exiting the glenohumeral joint and passing through the bicipital groove, the LHBT is supported and stabilized by a complex termed the biceps pulley, comprised of fibers from the superior glenohumeral ligament (SGHL), coracohumeral ligament (CHL), and (important to this article) fibers of the supraspinatus and subscapularis tendons. This complex forms a sling around the LHBT to help maintain the anatomical positioning of the tendon, particularly opposing anterior shearing stress and preventing anteromedial displacement.7,11,17,71
The coracohumeral ligament (CHL) is the most superficial layer of the biceps pulley mechanism and extends over the subscapularis (SScT) and supraspinatus (SST) tendons. The superior glenohumeral ligament fuses with the CHL laterally and forms a ligament layer between the biceps tendon (BT) and the superior-most inserting subscapularis tendon (SScT) at the lesser tuberosity (LT).
Image from: Werner A, Mueller T, Boehm D, Gohlke F. The stabilizing sling for the long head of the biceps tendon in the rotator cuff interval. A histoanatomic study. Am J Sports Med. 2000;28(1):28-31
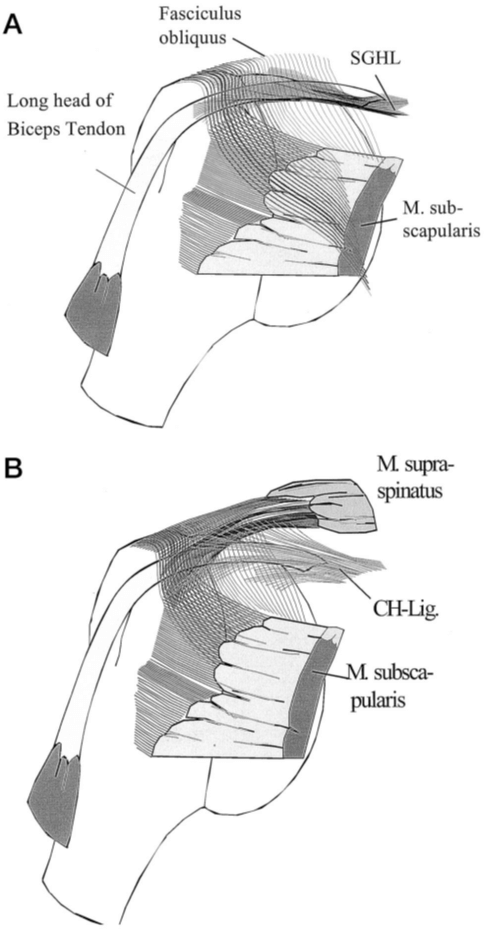
This displays:
- The interconnectivity of the tendons and ligaments more accurately than the previous image.
- The sharp angulation the LHB tendon makes when entering the bicipital groove.
According to several retrospective analyses, damage of the supraspinatus and/or subscapularis tendon(s) is strongly correlated to biceps pulley tears as well as subsequent LHB tendon pathologies. Rates as high as 75%-85% of cases with partial or full thickness subscapularis tears exhibit evidence of biceps pulley damage, and in such instances, it has been reported that as large as 75-90% of the biceps tendons have been shown to be either subluxed, dislocated, or completely torn.7,9,11,25,27
Furthermore, in a study conducted by Walch et al. they found even stronger correlations between the tissues of interest. In non-traumatic conditions, the patients with subluxing biceps tendons had subscapularis lesions in 100% of the cases and supraspinatus tears in 88% of the cases. Dislocations over the lesser tuberosity occurred only in the presence of subscapularis damage and almost always with additional supraspinatus damage (95%).70
In order to understand this relationship, it may be best to study the images provided above. As can be visualized, the supraspinatus and subscapularis tendon each play integral roles in maintaining biceps tendon position. When the LHB tendon passes through the biceps pulley, it makes a sharp turn (35-40°) before entering the bicipital groove.66 This point of angulation represents a significant mechanical vulnerability, which requires external assistance for stabilization. Largely, this duty falls on the biceps pulley complex. So not only are the supraspinatus and subscapularis responsible for providing active stabilization of the biceps through contraction, they also serve a passive role in mechanical stability due to their integration into the biceps pulley itself. Thus, the stress imparted upon the biceps tendon is compounded when there is evident structural damage.
Aside from any pain or force generation concerns associated with compromised biceps pulleys in isolation, structural deficiencies may additionally expose the LHB tendon to external shear and compressive stresses. When there is damage to the biceps pulley, the involved tissues are susceptible to a phenomenon known as anteriorsuperior impingement (ASI). Unlike SAIS, which is considered an external impingement, ASI is considered a form of internal impingement because the undersurface of the reflection pulley and the subscapularis tendon become compressed within the GH joint itself.
Similar to SAIS, it is often debated whether or not the ASI process is a physiological norm or if it represents a pathological progression. However, there appears to be evidence that intimately associates biceps pulley integrity and the occurrence of this compression. Habermeyer et al. found that when comparing between shoulders with known biceps pulley lesions, the probability of ASI significantly raised in accordance to the extent of RC pathology. The risk ratio of ASI increased to 4.99 when there was documented subscapularis tendon damage, and this ratio jumped to 12.0 when there were both subscapularis and supraspinatus tears. Therefore, this discovery led the researchers to speculate a causative cascade of events. In the presence of biceps pulley tears, the group theorizes that the LHB becomes unstable along its intra-articular course. This instability may lead to medial subluxation and subsequent shear stress placed upon the biceps tendon. Furthermore, this positional fault, according to Habermeyer, may negate the tendon’s role as an anterior stabilizer of the humeral head. Thus, excessive translation may further compress the pulley and RC structures within the GH joint, driving this cyclical pathological state.27
In reference to external factors, a third consideration involves the morphological changes that occur to the biceps tendon when exposed to excessive levels of stress. Multiple studies have found significant enlargement of the LHB tendon when comparing between patients presenting with and without rotator cuff dysfunction.8,58 This observation further insinuates the rotator cuff’s potential causative role in the development of biceps tendinopathy, as tendon thickening is a hallmark feature in pathological tendons.18b Although this adaptation is thought to be beneficial, the protective compensation can have detrimental repercussions if this occurs intra-articularly. Boileau and his colleagues coined the term “hourglass biceps” to describe a specific phenomenon where the intra-articular portion of the LHB tendon hypertrophies and creates an unwanted size discrepancy between the tendon and the bicipital groove. If the condition advances, the tendon can hypertrophy to an extent where it becomes entrapped within the joint when reaching overhead.5
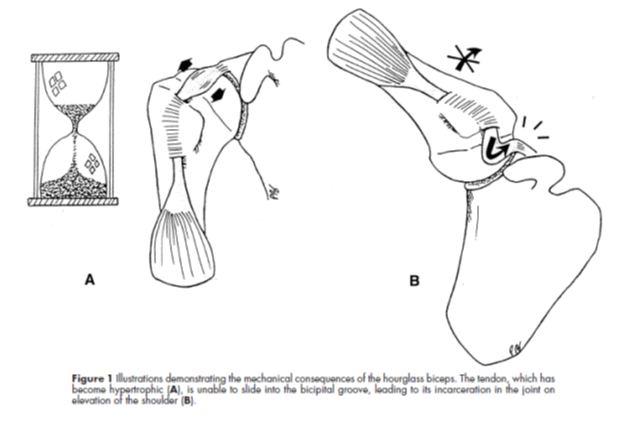
Figure 1 from Boileau5: Illustrations demonstrating the mechanical consequences of the hourglass biceps. The tendon which has become hypertrophic (A) is unable to slide into the bicipital groove, leading to its incarceration in the joint on elevation of the shoulder (B).
Of note, Boileau’s phenomenon was observed in patients with an average age of 62 with full-thickness rotator cuff tears.5 So while this drastic entrapment is unlikely to occur in this article’s target audience, this process may still have important implications. Chronic tendon adaptations due to excessive loading might lead to relative stenosis of the LHB tendon within the bicipital groove. This narrowing may impart external stress to the tendon and serve to presumptively hasten the degenerative progression.
Finally, rotator cuff insufficiency may impact the biceps tendon indirectly by influencing the surrounding synovial sheath. Since the sheath of the biceps tendon is continuous with the GH joint synovium, any joint pathology may simultaneously influence the tendon covering. Therefore, any inflammatory condition directly involving the shoulder joint can contribute to bicipital peritendinous effusion (BPE). Importantly, tissues that are intimately associated with the GH joint capsule (such as the rotator cuff) can also play a pivotal role in this regard. Symptomatic RC tears have been strongly linked to inflammatory changes within the joint synovium and have subsequently been correlated to the presence of BPE.1,8b,8c,52b,60b Aside from an independent source of pain, synovial inflammation (synovitis) has been proposed to lead to adhesion and scar formation, which would contribute to relative stenosis of the LHB tendon.67 This progression would impact the LHB tendon tissue quality much in the same way as the hourglass biceps phenomenon described above. Although this rationale appears sound in theory, the relationship appears tenuous in reality. When assessing patients with chronic LHB tendon pathologies, there is no evidence of acute or chronic inflammation, and the presence and extent of BPE (as well as tendon sheath characteristics) show low to no correlation to shoulder pain.52b,62b,65 Thus, when assessing the data in totality, no strong conclusions can be made regarding this impact at present.
So What?
At this point, it should become clear that the described internal and external mechanisms of biceps tendon degeneration, influenced by rotator cuff function, are not mutually exclusive from one another. Each external factor that places the involved tendon under duress can induce internal adaptations. Consequently, with reduced mechanical capacity due to said adaptations, there is likely greater instability and subsequent external stress placed upon the biceps. This problematic cycle highlights the importance of addressing not only the physiological characteristics of the primary tendon of interest, but also any contributing factors that may be chronically perpetuating the excessive loads.
Now that the relationship between RC and LHB pathologies has been established, the intuitive question becomes: If, and to what extent, can this process be altered. On this front, there is good and bad news to report. In regards to the structural adaptations noted above (biceps tendon hypertrophy, integrity loss of the RC tendon and/or biceps pulley), there is little to no evidence suggesting these qualities can be meaningfully influenced.7c,13b,18b Additionally, current evidence suggests there is minimal to no difference in total excursion of the humeral head within the glenoid cavity following therapeutic interventions.4,49 Meaning, if SAIS does indeed impact the RC and the LHB tendons, we may not have an adequate solution to combat the phenomenon.
Fortunately, the good news is that unless these changes are severe, it likely doesn’t matter. While I have exhaustively highlighted various anatomical correlations above, the mere presence of any of these abnormalities does not guarantee anything. Prevalence data indicates rotator cuff tears are present in up to 39% of ASYMPTOMATIC individuals.58b While there are correlations between underlying tissue quality and pain, with prospective studies indicating those with structural pathologies are more likely to subsequently develop symptoms, the discrepancy between physical state and pain is quite clear13b,58b. A point which cannot be emphasized enough is the disconnect between pain perception and tissue damage. The contention that pain is directly proportional to the current state of the involved tissue is inaccurate and fails to account for the complex nature of the phenomenon. Pain is now largely considered a perceptual output of the brain that is formed through a dynamic interaction between the individual and their environment. The resulting experience of pain is modulated based on knowledge, beliefs, and culture and is often poorly correlated to tissue characteristics.69b There are substantial changes that occur peripherally (at the local site of the involved tissue) and centrally (spinal cord and brain) following injuries, which can be influenced without requiring any specific adaptations to occur within the degenerative tendon (Pelletier, Cooper). Thus, those who have a known compromise of their RC or LHB tendons shouldn’t view their condition as an inevitable, unyielding progression of dysfunction and pain. Exploring this concept further would extend this already drawn out article, so I recommend anyone interested in this topic to reference the works of Lorimer Moseley here or Louis Gifford here for a good entry point into pain science.
Rotator Cuff Training
Finally to the part that people actually care about: how we intervene. When assessing outcomes from a broad perspective, current literature indicates positive changes are possible in a wide array of conditions. Diverse patient populations, with various duration and extent of rotator cuff tendon damage, are capable of successful rehab.39 Even in the presence of full-thickness tears, meaningful impact on kinematics is possible. This success is directly evidenced by Miller’s 2016 study, which examined dynamic intra-articular control in a population with known supraspinatus tears.49 Visually depicted in the image below, the data revealed a 36% reduction in humeral head motion following 12 weeks of exercise therapy.

Representative contact path kinematics for a single patient before therapy (A) and after therapy (B). The contact center is represented by a black circle, and the path followed by the contact center throughout the range of abduction is represented by the white line.
Similar studies have corroborated the above outcomes, improving confidence in the capacity to meaningfully alter internal movement.4 What becomes apparent is that in each scenario, on average, patients displayed an insufficiency in humeral control that was modifiable by exercise.4,49 If more precise intra-articular control is granted following intervention, there may be significant implications for the supplemental tissue(s) previously tasked with this role. As such, the internal demands placed upon the biceps tendon may be lessened.
When determining appropriate stress application and progression, it is important to first consider the current capacity of the tissue. If there is extreme sensitivity to loading, it may even require starting with low-intensity isometric contractions to build stress tolerance. This approach serves as a great entry point, as studies have found improved force expression, less pain, and reduced levels of cortical inhibition immediately following performance of sustained isometric contractions.54b Although these effects are less certain when discussing tendons of the upper body, it remains that exposing the tissue to tolerable levels of stress is beneficial from physiological and psychological standpoints.
Side Note: If this even remotely reflects your current capabilities, I implore you to seek medical advice.
Once load tolerance is established, rehabilitation is relatively simple. A recent systematic review demonstrated that inclusion of resistance exercise was a primary factor associated with positive outcomes; yet, specific recommendations regarding exercise volume, frequency, and intensity are not clear.39 This makes sense, as there is large heterogeneity between individuals presenting with rotator cuff dysfunction, rendering any notion of a universal “optimal” protocol obsolete. Recent evidence additionally suggests we may not need to be overly concerned with the specific selection and implementation of exercise interventions. Exercise interventions tailored to the particular deficiencies in patients presenting with SAIS have not been demonstrated to be more effective than general exercise programs when assessing pain, range of motion, strength, or function (Shire). Thus, as of now, it appears the best advice is to challenge the cuff sufficiently, with adequate volume, without evoking an adverse response.
Adam Meakins (a physiotherapist out of the UK) has put together several beneficial resources for management of rotator cuff disorders (see here and here for a quick list of common, effective exercises to perform). And for the minimalists reading this article, Dr. Chris Littlewood may have simplified this process even further. His group found similar (positive) results when comparing standard physical therapy treatment to a self-managed group who only used a single exercise.39b Over the course of 12 weeks, individuals performed one exercise for three sets of 10-15 repetitions twice per day. The exercise chosen (either abduction or external rotation) progressed from an isometric contraction, to a resisted isotonic contraction of the same movement, to a resisted, compound movement (push-up or pull-up). The intensity was to be adjusted such that it MUST PROVOKE PAIN during the performance, with no evidence of worsening of symptoms upon cessation. This is a vital stipulation for several reasons. First, the pain provocation helps indicate that certain thresholds of stress are being applied to the appropriate tissue- thus helping to promote any physiological adaptations within the shoulder itself. Second, resilience in spite of symptoms improves self-efficacy while simultaneously helping to psychologically condition an individual away from harmful interpretations of their current state. The authors are adamant that maintaining an optimistic perception of the pathology is an essential component of successful rehabilitation. Inaccurate appraisal of symptom meaning (i.e. that pain equates to tissue damage) may lead to destructive, self-perpetuation of the condition due to fear-avoidance tendencies.
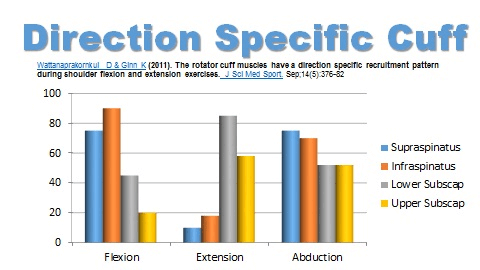
Finally, when training for performance, certain provisions should probably still be in place to protect rotator cuff health. As shown in a recent study by Wattanaprakornkul et al, the rotator cuff musculature displays distinct activation patterns specific to the direction of resistance.70b Flexion exercises lead to greater EMG activity of the posterior musculature (supraspinatus, infraspinatus), extension exercises lead to greater EMG activity of the anterior musculature (subscapularis), and abduction exercises lead to relatively similar levels of activity globally.
Data originally from Wattanaprakornkul70b, Image provided by Adam Meakins here
This specific activation pattern indicates the importance of maintaining balance in a training program. I recommend calculating the average total volume performed in each direction to see if any discrepancies exist. From there, it would be wise to build capacity of the rotator cuff through isolated training and integrated stabilization exercises. Quinn Henoch has several excellent videos covering higher level training for shoulder function (example here), and his channel offers value for those seeking more in-depth philosophy and application of rehab principles into barbell sports.
Summing Up
One of the best parts about being a physical therapist is helping people continue to do the things they value. When faced with injury, lifters often fixate on the movements they can no longer tolerate instead of the options they can perform successfully. Often, this pessimistic focus is unnecessary, as we can alter rather than abandon. Intelligent program design, individually molded based upon the physical characteristics and the specific goals of the lifter, is extremely important. As discussed (in way too much detail), simple changes can be made to primary, secondary, and accessory lifts that allow for the LHB tendon to settle down (and potentially adapt) while still making progress toward competitive goals. Finally, with the knowledge as to why these injuries may be occurring, the risk of further degenerative progression may be influenced. Hopefully, this article provided the valuable insight needed to navigate this condition and allow for you, or those you work with clinically, to remain on the platform as long as desired.
Acknowledgements
I’ve surrounded myself with a couple of smart friends who hold me accountable. Thanks to Scot Morrison, Derek Miles, Ricky Tapia, and Dan Raimondi for all the help regarding content. Big thanks to my brother Stephen Eure and Greg’s amazing wife Lyndsey for help with general editing. And of course Greg for giving me a platform to reach others.
References
1. Abrams, G., Luria, A., Carr, R., Rhodes, C., Robinson, W., & Sokolove, J. (2016). Association of synovial inflammation and inflammatory mediators with glenohumeral rotator cuff pathology. Journal Of Shoulder And Elbow Surgery, 25(6), 989-997. http://dx.doi.org/10.1016/j.jse.2015.10.011
1b. Ackland, David C., and Marcus G. Pandy. “Moment Arms Of The Shoulder Muscles During Axial Rotation”. Journal Of Orthopaedic Research, vol 29, no. 5, 2010, pp. 658-667. Wiley-Blackwell, doi:10.1002/jor.21269
2. Ackland, D. C., & Pandy, M. G. (2009). Lines of action and stabilizing potential of the shoulder musculature. Journal of Anatomy, 215(2), 184–197. doi:10.1111/j.1469-7580.2009.01090.x
3. Barrett, Eva et al. “Is Thoracic Spine Posture Associated With Shoulder Pain, Range Of Motion And Function? A Systematic Review”. Manual Therapy, vol 26, 2016, pp. 38-46. Elsevier BV, doi:10.1016/j.math.2016.07.008
4. Baumer, T. G., Chan, D., Mende, V., Dischler, J., Zauel, R., van Holsbeeck, M., … Bey, M. J. (2016). Effects of Rotator cuff pathology and physical therapy on in vivo shoulder motion and clinical outcomes in patients with a symptomatic full-thickness Rotator cuff tear. Orthopaedic Journal of Sports Medicine, 4(9), doi:10.1177/2325967116666506
5. Boileau, P., Ahrens, P. M., & Hatzidakis, A. M. (2004). Entrapment of the long head of the biceps tendon: The hourglass biceps—a cause of pain and locking of the shoulder. Journal of Shoulder and Elbow Surgery, 13(3), 249–257. doi:10.1016/j.jse.2004.01.001
5b. Bohm S, Mersmann F, Arampatzis A. Human tendon adaptation in response to mechanical loading: a systematic review and meta-analysis of exercise intervention studies on healthy adults. Sports Med Open. 2015;1(1):7
6. Braman, Jonathan P. et al. “In Vivo Assessment Of Scapulohumeral Rhythm During Unconstrained Overhead Reaching In Asymptomatic Subjects”. Journal Of Shoulder And Elbow Surgery, vol 18, no. 6, 2009, pp. 960-967. Elsevier BV, doi:10.1016/j.jse.2009.02.001.
7. Braun, S., Horan, M. P., Elser, F., & Millett, P. J. (2011). Lesions of the biceps pulley. The American Journal of Sports Medicine, 39(4), 790–795. doi:10.1177/0363546510393942
7b. Brossmann, J., Preidler, K., Pedowitz, R., White, L., Trudell, D., & Resnick, D. (1996). Shoulder impingement syndrome: influence of shoulder position on rotator cuff impingement–an anatomic study. American Journal Of Roentgenology, 167(6), 1511-1515. http://dx.doi.org/10.2214/ajr.167.6.8956588
7c. Camargo, P. (2014). Eccentric training as a new approach for rotator cuff tendinopathy: Review and perspectives. World Journal Of Orthopedics, 5(5), 634. http://dx.doi.org/10.5312/wjo.v5.i5.634
8. Chang, K., Chen, W., Wang, T., Hung, C., & Chien, K. (2014). Quantitative Ultrasound Facilitates the Exploration of Morphological Association of the Long Head Biceps Tendon with Supraspinatus Tendon Full Thickness Tear. PLoS ONE,9(11). doi:10.1371/journal.pone.0113803
8b. Chang, Ke-Vin et al. “Associations Of Sonographic Abnormalities Of The Shoulder With Various Grades Of Biceps Peritendinous Effusion (BPE)”. Ultrasound In Medicine & Biology, vol 40, no. 2, 2014, pp. 313-321. Elsevier BV, doi:10.1016/j.ultrasmedbio.2013.10.002.
8c. Chang, Ke-Vin et al. “Association Of Bicipital Peritendinous Effusion With Subacromial Impingement: A Dynamic Ultrasonographic Study Of 337 Shoulders”. Scientific Reports, vol 6, no. 1, 2016, Springer Nature, doi:10.1038/srep38943.
9. Chen, C.-H., Hsu, K.-Y., Chen, W.-J., & Shih, C.-H. (2005). Incidence and severity of biceps Long Head Tendon lesion in patients with complete Rotator cuff tears. The Journal of Trauma: Injury, Infection, and Critical Care, 58(6), 1189–1193. doi:10.1097/01.ta.0000170052.84544.34
10. Chen, C.-H., Chang, C.-H., Su, C.-I., Wang, K.-C., Wang, I.-C., Liu, H.-T., … Hsu, K.-Y. (2012). Classification and analysis of pathology of the long head of the biceps tendon in complete rotator cuff tears. Biomedical Journal, 35(3), 263. doi:10.4103/2319-4170.106145
11. Choi, C. H., Kim, S. S., & Lee, J. H. (2015). Arthroscopic changes of the biceps pulley in Rotator cuff tear and its clinical significance in relation to treatment. Clinics in Orthopedic Surgery, 7(3), 365. doi:10.4055/cios.2015.7.3.365
12. Cook J, Docking S “Rehabilitation will increase the ‘capacity’ of your …insert musculoskeletal tissue here….” Defining ‘tissue capacity’: a core concept for clinicians Br J Sports Med Published Online First: 08 August 2015. doi: 10.1136/bjsports-2015-094849
13. Cook, J., & Purdam, C. (2011). Is compressive load a factor in the development of tendinopathy? British Journal of Sports Medicine, 46(3), 163–168. doi:10.1136/bjsports-2011-090414
13b. Cook JL, Rio E, Purdam CR, Docking SI. Revisiting the continuum model of tendon pathology: what is its merit in clinical practice and research?. Br J Sports Med. 2016
14. Cools, Ann M. et al. “Evidence-Based Rehabilitation Of Athletes With Glenohumeral Instability”. Knee Surgery, Sports Traumatology, Arthroscopy, vol 24, no. 2, 2015, pp. 382-389. Springer Nature, doi:10.1007/s00167-015-3940-x
15. Cools AM, Borms D, Cottens S, Himpe M, Meersdom S, Cagnie B. Rehabilitation exercises for athletes with biceps disorders and SLAP lesions: A continuum of exercises with increasing loads on the biceps. The American Journal of Sports Medicine. 2014;42(6):1315–1322. doi:10.1177/0363546514526692
16. Cutts, Steven et al. “Anterior Shoulder Dislocation”. The Annals Of The Royal College Of Surgeons Of England, vol 91, no. 1, 2009, pp. 2-7. Royal College Of Surgeons Of England, doi:10.1308/003588409×359123
17. Ditsios, K., Agathangelidis, F., Boutsiadis, A., Karataglis, D., & Papadopoulos, P. (2012). Long Head of the biceps pathology combined with Rotator cuff tears. Advances in Orthopedics, 2012, 1–6. doi:10.1155/2012/405472
18. Docking, S. (2013). Relationship between compressive loading and ECM changes in tendons. Muscles, Ligaments and Tendons Journal. doi:10.11138/mltj/2013.3.1.007
18b. Docking SI, Cook J. Pathological tendons maintain sufficient aligned fibrillar structure on ultrasound tissue characterization (UTC). Scand J Med Sci Sports. 2016;26(6):675-83
18c. Earp JE, Newton RU, Cormie P, Blazevich AJ. Faster Movement Speed Results in Greater Tendon Strain during the Loaded Squat Exercise. Front Physiol. 2016;7:366
19. Elser, F., Braun, S., Dewing, C. B., Giphart, J. E., & Millett, P. J. (2011). Anatomy, function, injuries, and treatment of the Long Head of the biceps brachii Tendon. Arthroscopy: The Journal of Arthroscopic & Related Surgery, 27(4), 581–592. doi:10.1016/j.arthro.2010.10.014
20. Eshuis, Rienk, and Arthur De Gast. “Role Of The Long Head Of The Biceps Brachii Muscle In Axial Humeral Rotation Control”. Clinical Anatomy, vol 25, no. 6, 2011, pp. 737-745. Wiley-Blackwell, doi:10.1002/ca.22001
21. Factor, D., & Dale, B. (2014). CURRENT CONCEPTS OF ROTATOR CUFF TENDINOPATHY. International Journal of Sports Physical Therapy, 9(2), 274–288
22. Farias, D. D., Willardson, J. M., Paz, G. A., Bezerra, E. D., & Miranda, H. (2016). Maximal strength performance and muscle activation for the bench press and triceps extension exercises adopting dumbbell, barbell and machine modalities over multiple sets. Journal of Strength and Conditioning Research, 1. doi:10.1519/jsc.0000000000001651
23. Friedman, D. J., Dunn, J. C., Higgins, L. D., & Warner, J. J. P. (2008). Proximal biceps Tendon. Sports Medicine and Arthroscopy Review, 16(3), 162–169. doi:10.1097/jsa.0b013e318184f549
24. Giphart, J. E., Elser, F., Dewing, C. B., Torry, M. R., & Millett, P. J. (2011). The Long Head of the biceps Tendon has minimal effect on in vivo Glenohumeral Kinematics: A biplane Fluoroscopy study. The American Journal of Sports Medicine, 40(1), 202–212. doi:10.1177/0363546511423629
25. Godenèche, A., Object, object, Nové-Josserand, L., Audebert, S., Toussaint, B., Denard, P. J., & Lädermann, A. (2016). Relationship between subscapularis tears and injuries to the biceps pulley. Knee Surgery, Sports Traumatology, Arthroscopy. doi:10.1007/s00167-016-4374-9
26. Gong, Wontae et al. “An Analysis Of The Correlation Between Humeral Head Anterior Glide Posture And Elbow Joint Angle, Forward Head Posture And Glenohumeral Joint Range Of Motion”. Journal Of Physical Therapy Science, vol 25, no. 4, 2013, pp. 489-491. Society Of Physical Therapy Science, doi:10.1589/jpts.25.489
27. Habermeyer, P., Magosch, P., Pritsch, M., Scheibel, M. T., & Lichtenberg, S. (2004). Anterosuperior impingement of the shoulder as a result of pulley lesions: A prospective arthroscopic study. Journal of Shoulder and Elbow Surgery, 13(1), 5–12. doi:10.1016/j.jse.2003.09.013
28. Huegel, J., Williams, A. A., & Soslowsky, L. J. (2014). Rotator cuff biology and Biomechanics: A review of normal and pathological conditions. Current Rheumatology Reports, 17(1), . doi:10.1007/s11926-014-0476-x
29. Khan, K M, and A Scott. “Mechanotherapy: How Physical Therapists’ Prescription Of Exercise Promotes Tissue Repair”. British Journal Of Sports Medicine, vol 43, no. 4, 2009, pp. 247-252. BMJ, doi:10.1136/bjsm.2008.054239
30. Kido, T., Itoi, E., Konno, N., Sano, A., Urayama, M., & Sato, K. (1998). Electromyographic activities of the biceps during arm elevation in shoulders with rotator cuff tears. Acta Orthopaedica Scandinavica, 69(6), 575–579. doi:10.3109/17453679808999258
31. Kolber, Morey J et al. “Shoulder Injuries Attributed To Resistance Training: A Brief Review”. Journal Of Strength And Conditioning Research, vol 24, no. 6, 2010, pp. 1696-1704. Ovid Technologies (Wolters Kluwer Health), doi:10.1519/jsc.0b013e3181dc4330
32. Kuhn, John E. et al. “External Rotation Of The Glenohumeral Joint: Ligament Restraints And Muscle Effects In The Neutral And Abducted Positions”. Journal Of Shoulder And Elbow Surgery, vol 14, no. 1, 2005, pp. S39-S48. Elsevier BV, doi:10.1016/j.jse.2004.09.016.
33. Kurdziel, M. D., Moravek, J. E., Wiater, B. P., Davidson, A., Seta, J., Maerz, T., … Wiater, J. M. (2015). The impact of rotator cuff deficiency on structure, mechanical properties, and gene expression profiles of the long head of the biceps tendon (LHBT): Implications for management of the LHBT during primary shoulder arthroplasty. Journal of Orthopaedic Research, 33(8), 1158–1164. doi:10.1002/jor.22895
34. Kwak, A., Poplawski, S., & Stevens, K. (2012). The biceps muscle from shoulder to elbow. Seminars in Musculoskeletal Radiology, 16(04), 296–315. doi:10.1055/s-0032-1327004
35. Lakemeier, S., Reichelt, J. J., Timmesfeld, N., Fuchs-Winkelmann, S., Paletta, J. R., & Schofer, M. D. (2010). The relevance of long head biceps degeneration in the presence of rotator cuff tears. BMC Musculoskeletal Disorders, 11(1), . doi:10.1186/1471-2474-11-191
36. Landin, D., Myers, J., Thompson, M., Castle, R., & Porter, J. (2008). The role of the biceps brachii in shoulder elevation. Journal of Electromyography and Kinesiology, 18(2), 270–275. doi:10.1016/j.jelekin.2006.09.012
37. Lavagnino, M., Arnoczky, S. P., Elvin, N., & Dodds, J. (2008). Patellar Tendon strain is increased at the site of the jumper’s knee lesion during knee Flexion and Tendon loading: Results and Cadaveric testing of a computational model. The American Journal of Sports Medicine, 36(11), 2110–2118. doi:10.1177/0363546508322496
38. Levy, A. S., Kelly, B. T., Lintner, S. A., Osbahr, D. C., & Speer, K. P. (2001). Function of the long head of the biceps at the shoulder: Electromyographic analysis. Journal of Shoulder and Elbow Surgery, 10(3), 250–255. doi:10.1067/mse.2001.113087
39. Littlewood, C., Malliaras, P., & Chance-Larsen, K. (2015). Therapeutic exercise for rotator cuff tendinopathy. International Journal of Rehabilitation Research, 38(2), 95–106. doi:10.1097/mrr.0000000000000113
39b. Littlewood, C., Malliaras, P., Mawson, S., May, S., & Walters, S. (2014). Self-managed loaded exercise versus usual physiotherapy treatment for rotator cuff tendinopathy: a pilot randomised controlled trial. Physiotherapy, 100(1), 54-60. http://dx.doi.org/10.1016/j.physio.2013.06.001
40. Ludewig, Paula M., and Jonathan P. Braman. “Shoulder Impingement: Biomechanical Considerations In Rehabilitation”. Manual Therapy, vol 16, no. 1, 2011, pp. 33-39. Elsevier BV, doi:10.1016/j.math.2010.08.004
41. Ludewig PM, Reynolds JF. The association of Scapular Kinematics and Glenohumeral joint Pathologies. Journal of Orthopaedic & Sports Physical Therapy. 2009;39(2):90–104. doi:10.2519/jospt.2009.2808
42. McFarland EG, Maffulli N, Del Buono A, Murrell GA, Garzon-Muvdi J, Petersen SA. Impingement is not impingement: the case for calling it “Rotator Cuff Disease”.Muscles Ligaments Tendons J. 2013;3:196–200.
43. Mackenzie, T. A., Herrington, L., Funk, L., Horsley, I., & Cools, A. (2016). Relationship between extrinsic factors and the acromio-humeral distance. Manual Therapy, 23, 1–8. doi:10.1016/j.math.2016.02.005
44. Mackenzie, T. A., Herrington, L., Horlsey, I., & Cools, A. (2015). An evidence-based review of current perceptions with regard to the subacromial space in shoulder impingement syndromes: Is it important and what influences it? Clinical Biomechanics, 30(7), 641–648. doi:10.1016/j.clinbiomech.2015.06.001
44b. Magnusson SP, Langberg H, Kjaer M. The pathogenesis of tendinopathy: balancing the response to loading. Nat Rev Rheumatol. 2010;6(5):262-8
45. Malliaras, Peter et al. “Patellar Tendinopathy: Clinical Diagnosis, Load Management, And Advice For Challenging Case Presentations”. Journal Of Orthopaedic & Sports Physical Therapy, vol 45, no. 11, 2015, pp. 887-898. Journal Of Orthopaedic & Sports Physical Therapy (JOSPT), doi:10.2519/jospt.2015.5987
46. Mandalidis, D. et al. “Electromyographic Activity Of The Biceps Brachii During Maximal Voluntary Rotation Of The Abducted Shoulder”. The Open Sports Medicine Journal, vol 2, no. 1, 2008, pp. 69-74. Bentham Science Publishers Ltd., doi:10.2174/1874387000802010069.
47. Massimini, Daniel F et al. “In-Vivo Glenohumeral Translation And Ligament Elongation During Abduction And Abduction With Internal And External Rotation”. Journal Of Orthopaedic Surgery And Research, vol 7, no. 1, 2012, p. 29. Springer Nature, doi:10.1186/1749-799x-7-29
48. McQuade, K. J. et al. “Critical And Theoretical Perspective On Scapular Stabilization: What Does It Really Mean, And Are We On The Right Track?”. Physical Therapy, vol 96, no. 8, 2016, pp. 1162-1169. Oxford University Press (OUP), doi:10.2522/ptj.20140230
49. Miller RM, Popchak A, Vyas D, et al. Effects of exercise therapy for the treatment of symptomatic full-thickness supraspinatus tears on in vivo glenohumeral kinematics. Journal of Shoulder and Elbow Surgery. 2016;25(4):641–649. doi:10.1016/j.jse.2015.08.048
50. Millett PJ, Giphart JE, Wilson KJ, Kagnes K, Greenspoon JA. Alterations in Glenohumeral Kinematics in patients with Rotator cuff tears measured with biplane Fluoroscopy. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2016;32(3):446–451. doi:10.1016/j.arthro.2015.08.031
50b. Morton RW, Oikawa SY, Wavell CG, et al. Neither load nor systemic hormones determine resistance training-mediated hypertrophy or strength gains in resistance-trained young men. J Appl Physiol. 2016;121(1):129-38
51. Nacimento VYS, Torres RJB, Beltrão NB, et al. Shoulder muscle activation levels during exercises with axial and rotational load on stable and unstable surfaces. Journal of Applied Biomechanics. October 2016:1–20. doi:10.1123/jab.2016-0177
52. Nho, S. J., Strauss, E. J., Lenart, B. A., Provencher, M. T., Mazzocca, A. D., Verma, N. N., & Romeo, A. A. (2010). Long Head of the biceps Tendinopathy: Diagnosis and management. American Academy of Orthopaedic Surgeon, 18(11), 645–656. doi:10.5435/00124635-201011000-00002
52b. Park, In et al. “Evaluation Of The Effusion Within Biceps Long Head Tendon Sheath Using Ultrasonography”. Clinics In Orthopedic Surgery, vol 7, no. 3, 2015, p. 351. The Korean Orthopaedic Association (KAMJE), doi:10.4055/cios.2015.7.3.351.
53. Pimentel, Iago et al. “Smith Machine vs. Barbell: Ten Repetition Maximum Loads and Muscle Activation Pattern during Upper Body Exercises”. Journal Of Exercise Physiology Online, vol 19, no. 5, 2016, pp. 86-92.
53b. Post, M., & Benca, P. (1989). Primary Tendinitis of the Long Head of the Biceps. Clinical Orthopaedics And Related Research, &NA;(246), 117???125. http://dx.doi.org/10.1097/00003086-198909000-00019
53c. Pufe, T., Petersen, W., Mentlein, R., & Tillmann, B. (2005). The role of vasculature and angiogenesis for the pathogenesis of degenerative tendons disease. Scandinavian Journal Of Medicine And Science In Sports, 15(4), 211-222. http://dx.doi.org/10.1111/j.1600-0838.2005.00465.x
54. Redondo-Alonso, L., Chamorro-Moriana, G., Jiménez-Rejano, J. J., López-Tarrida, P., & Ridao-Fernández, C. (2014). Relationship between chronic pathologies of the supraspinatus tendon and the long head of the biceps tendon: Systematic review. BMC Musculoskeletal Disorders, 15(1), . doi:10.1186/1471-2474-15-377
54b. Rio E, Kidgell D, Purdam C, et al. Isometric exercise induces analgesia and reduces inhibition in patellar tendinopathy. Br J Sports Med. 2015;49(19):1277-83
54c. Roberts TJ, Konow N. How tendons buffer energy dissipation by muscle. Exerc Sport Sci Rev. 2013;41(4):186-93
55. Saeterbakken AH, Fimland MS. Electromyographic activity and 6RM strength in bench press on stable and unstable surfaces. J Strength Condit Res. 2013; 27(4):1101±7
56. Saeterbakken, Atle H. et al. “A Comparison Of Muscle Activity And 1-RM Strength Of Three Chest-Press Exercises With Different Stability Requirements”. Journal Of Sports Sciences, vol 29, no. 5, 2011, pp. 533-538. Informa UK Limited, doi:10.1080/02640414.2010.543916.
57. Sahrmann SA: Diagnosis and treatment of movement impairment syndrome. St Louis: Mosby, 2002, pp 231–234.
58. Sakurai, G., Ozaki, J., Tomita, Y., Nakagawa, Y., Kondo, T., & Tamai, S. (1998). Morphologic changes in long head of biceps brachii in rotator cuff dysfunction. Journal of Orthopaedic Science, 3(3), 137–142. doi:10.1007/s007760050033
58b. Sambandam, S. (2015). Rotator cuff tears: An evidence based approach. World Journal Of Orthopedics, 6(11), 902. http://dx.doi.org/10.5312/wjo.v6.i11.902
59. Sarmento M. (2015). Long head of biceps: From anatomy to treatment. Acta Reumatologica Portuguesa, 40, 26-33
60. Seitz, A. L., McClure, P. W., Finucane, S., Boardman, N. D., & Michener, L. A. (2011). Mechanisms of rotator cuff tendinopathy: Intrinsic, extrinsic, or both? Clinical Biomechanics, 26(1), 1–12. doi:10.1016/j.clinbiomech.2010.08.001
60b. Shindle, M., Chen, C., Robertson, C., DiTullio, A., Paulus, M., & Clinton, C. et al. (2011). Full-thickness supraspinatus tears are associated with more synovial inflammation and tissue degeneration than partial-thickness tears. Journal Of Shoulder And Elbow Surgery, 20(6), 917-927. http://dx.doi.org/10.1016/j.jse.2011.02.015
61. Shire, Alison R. et al. “Specific Or General Exercise Strategy For Subacromial Impingement Syndrome–Does It Matter? A Systematic Literature Review And Meta Analysis”. BMC Musculoskeletal Disorders, vol 18, no. 1, 2017, Springer Nature, doi:10.1186/s12891-017-1518-0
62. Siewe, J. et al. “Injuries And Overuse Syndromes In Powerlifting”. International Journal Of Sports Medicine, vol 32, no. 09, 2011, pp. 703-711. Thieme Publishing Group, doi:10.1055/s-0031-1277207
62b. Singaraju, Vamsi M. et al. “Biceps Tendinitis In Chronic Rotator Cuff Tears: A Histologic Perspective”. Journal Of Shoulder And Elbow Surgery, vol 17, no. 6, 2008, pp. 898-904. Elsevier BV, doi:10.1016/j.jse.2008.05.044.
63. Spall, P., Ribeiro, D. C., & Sole, G. (2016). Electromyographic activity of shoulder girdle muscles in patients with symptomatic and asymptomatic Rotator cuff tears: A systematic review and Meta-Analysis. PM&R, 8(9), 894–906. doi:10.1016/j.pmrj.2016.02.015
64. Stastny P, Goøaś A, Blazek D, Maszczyk A, Wilk M, Pietraszewski P, et al. (2017) A systematic review of surface electromyography analyses of the bench press movement task. PLoS ONE 12(2): e0171632. doi:10.1371/journal.pone.0171632
65. Streit, Jonathan et al. “Tendinopathy Of The Long Head Of The Biceps Tendon: Histopathologic Analysis Of The Extra-Articular Biceps Tendon And Tenosynovium”. Open Access Journal Of Sports Medicine, 2015, p. 63. Dove Medical Press Ltd., doi:10.2147/oajsm.s76325
66. Taylor, S. A., & O’Brien, S. J. (2016). Clinically relevant anatomy and Biomechanics of the proximal biceps. Clinics in Sports Medicine, 35(1), 1–18. doi:10.1016/j.csm.2015.08.005
67. Taylor, Samuel A. et al. “The Anatomy And Histology Of The Bicipital Tunnel Of The Shoulder”. Journal Of Shoulder And Elbow Surgery, vol 24, no. 4, 2015, pp. 511-519. Elsevier BV, doi:10.1016/j.jse.2014.09.026
68. Tillaar R van den, Saeterbakken A. Effect of fatigue upon performance and Electromyographic activity in 6-RM bench press. Journal of Human Kinetics. 2014;40(1). doi:10.2478/hukin-2014-0007
69. Teunis, Teun et al. “A Systematic Review And Pooled Analysis Of The Prevalence Of Rotator Cuff Disease With Increasing Age”. Journal Of Shoulder And Elbow Surgery, vol 23, no. 12, 2014, pp. 1913-1921. Elsevier BV, doi:10.1016/j.jse.2014.08.001.
69b. Thacker, M. (2015). Louis Gifford – revolutionary: the Mature Organism Model, an embodied cognitive perspective of pain. Psychother. Priv. Pract.152, 4–9
70. Walch, G., Nové-Josserand, L., Boileau, P., & Levigne, C. (1998). Subluxations and dislocations of the tendon of the long head of the biceps. Journal of Shoulder and Elbow Surgery, 7(2), 100–108. doi:10.1016/s1058-2746(98)90218-x
70b. Wattanaprakornkul, D., Cathers, I., Halaki, M., & Ginn, K. (2011). The rotator cuff muscles have a direction specific recruitment pattern during shoulder flexion and extension exercises. Journal Of Science And Medicine In Sport, 14(5), 376-382. http://dx.doi.org/10.1016/j.jsams.2011.01.001
71. Werner A, Mueller T, Boehm D, Gohlke F. The stabilizing sling for the long head of the biceps tendon in the rotator cuff interval. A histoanatomic study. Am J Sports Med. 2000;28(1):28-31
71b. Wiesinger HP, Kösters A, Müller E, Seynnes OR. Effects of Increased Loading on In Vivo Tendon Properties: A Systematic Review. Med Sci Sports Exerc. 2015;47(9):1885-95
72. Yamaguchi, K., Riew, D., Galatz, L., Syme, J., & Neviaser, R. (1997). Biceps Activity During Shoulder Motion: An Electromyographic Analysis. Clinical Orthopaedics And Related Research, 336, 122-129. http://dx.doi.org/10.1097/00003086-199703000-00017
73. Zabrzyński, J., & Szumlański, A. (2016). Tendinopathy of the long head of the biceps tendon – physical examination confronted with shoulder arthroscopy findings. Medical and Biological Sciences, 30(2), 67. doi:10.12775/mbs.2016.008