Key points
- A muscle strain occurs when the strain energy the muscle is forced to absorb exceeds the strength of the tissue.
- Two-joint muscles are more susceptible to muscle strains, and nothing increases your likelihood of a strain more than a previous strain in the same muscle.
- Proper warm-ups, developing adequate mobility, and avoiding excessive fatigue decrease your risk of a muscle strain.
Background
Few things are more annoying than injuries. Your training is going well, then all of a sudden you’re laid up rehabbing some sort of sprain or strain for a few weeks or months.
Avoiding injuries while still training hard is a major key for consistent progress in the gym. But before you can know how to avoid injuries, you have to know why they happen in the first place.
This article addresses why one major class of injuries – muscle strains – happen in the first place.
Muscle injuries are classified as either direct or indirect. Direct injuries include things like bruises or gashes that occur as a result of some external force assaulting the muscle. Indirect injuries are those caused by muscle contraction itself, including functional disorders (like DOMS) and structural disorders (muscle fiber tears).
A muscle strain is an indirect, structural injury. They’re often referred to as “pulled” or “tweaked” muscles.
Strains come in varying degrees of severity, including “partial” (a few torn fibers), “subtotal” (a bunch of torn fibers, with some remaining intact), and “complete” (the entire muscle is ripped in two) [1].
Epidemiology & Significance
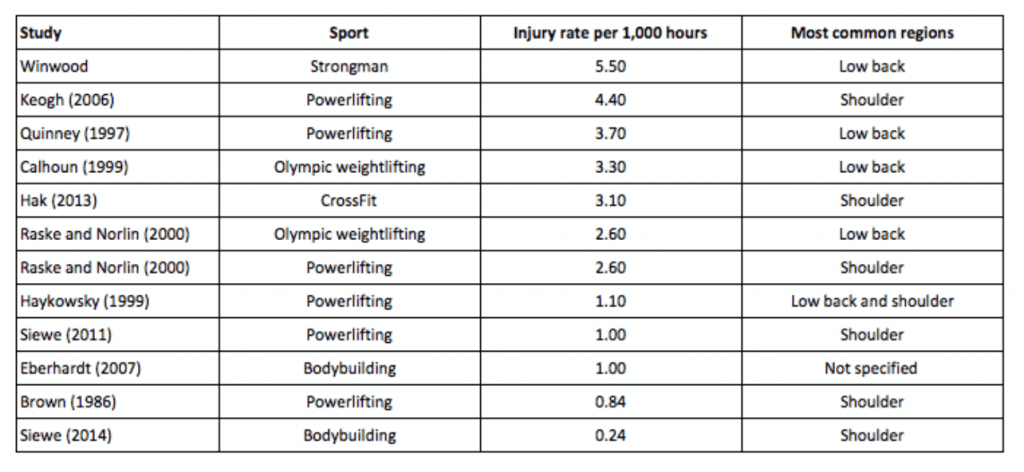
So, how common are injuries from strength training?
Anywhere from .24 to 5.5 per 1000 hours of training.
(image credit http://www.strengthandconditioningresearch.com/2014/07/08/injury-strength-sports/)
For comparison, strength athletes are injured about as often as people training for triathlons (1.9 injuries per 1000 hours), and generally less often than team sport athletes (from as low as 1.9 per 1000 hours for baseball practice to as high as 35.9 per 1000 hours for football games) [2-6, 34].
Acute muscle injuries rank as the most frequent type of trauma for athletes, accounting for a whopping one-fifth of all injuries. Of these injuries, acute muscle strains are among the most common [2,4].
Despite advancements in the scientific, medical, and athletic communities, incidence of injury has remained largely unchanged over the last 30 years.
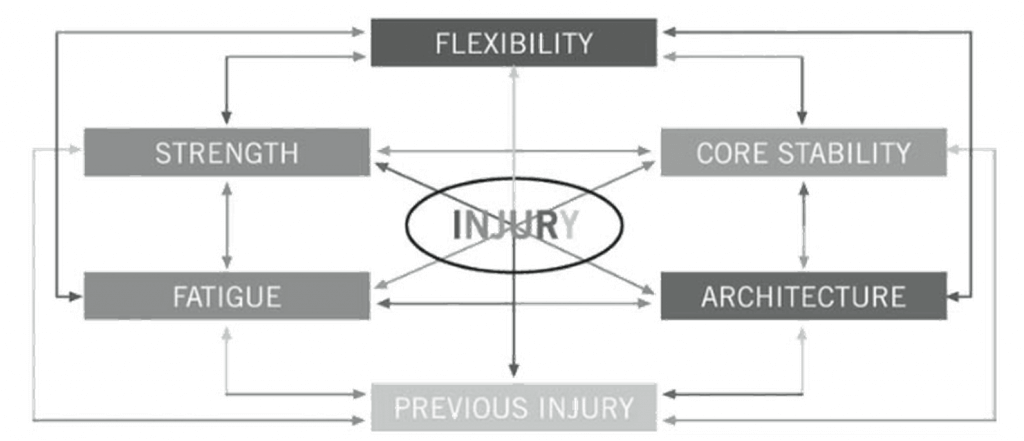
Conceptual model showing that, basically, muscle strain injuries are complicated [8]
Anatomy of the Muscle-tendon Unit
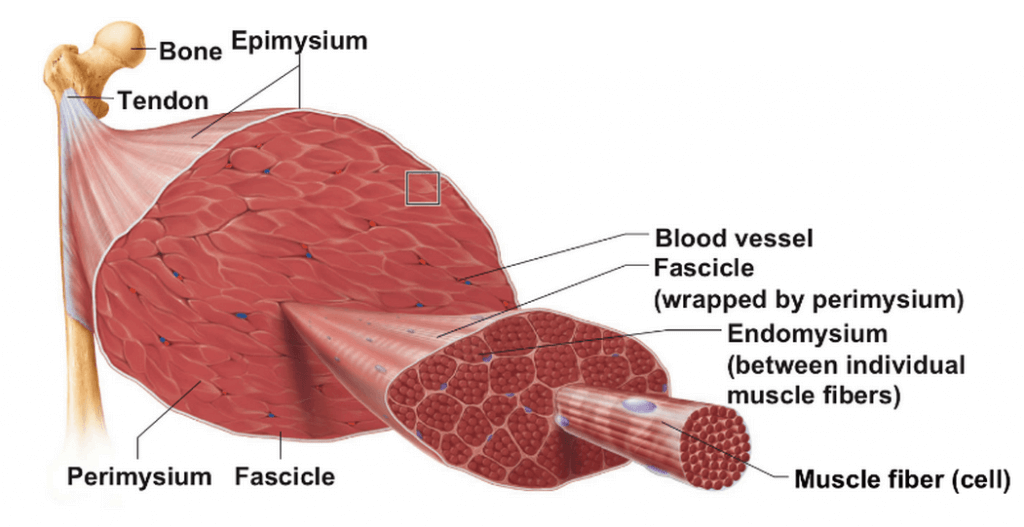
Human skeletal muscle consists of hundreds or even thousands of muscle fibers, nerve fibers, and blood vessels and accounts for approximately 40% of body mass [1]. Multiple layers of connective tissue wrappings encase these structures. Muscles produce movement of the skeleton via attachments directly on bone or via tendinous insertion [9].
Anatomy of muscle-tendon unit [9]
Whiting and Zernicke explain the role of skeletal muscle best:
Skeletal muscles are the engines that provide the human body with the power needed to move. They have a unique ability among all the body’s tissues to generate force and contract. Their specialized cells allow muscle to produce force (sometimes referred to as tension, or tensile load) and change their shape by contracting, or shortening. [10]
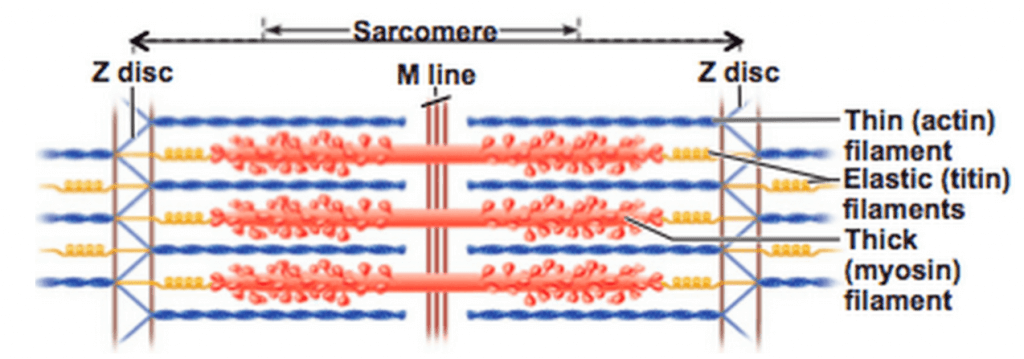
This process of contraction and force production is described by sliding filament theory. The smallest contractile unit of a muscle fiber is the sarcomere, which is composed of proteins that pull against each other, pulling the ends of the sarcomere closer together [9]. When that happens in a bunch of sarcomeres down the length of the entire muscle, voila! Muscle contraction.
Diagram of a sarcomere [9]
(Note: There’s an updated version of sliding filament theory known as winding filament theory, that helps better explain why a muscle can produce more force in an eccentric or isometric contraction than a concentric contraction [33]. However, that’s not overly important for our purposes here.)
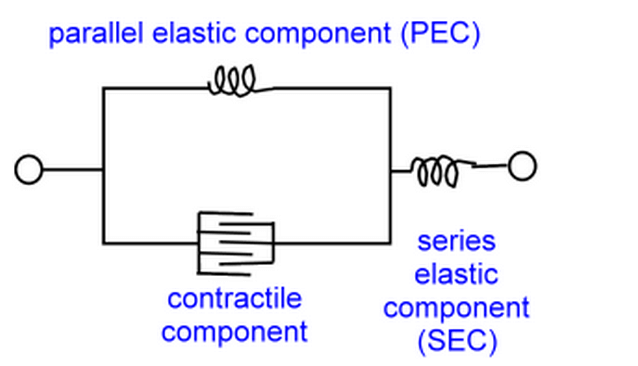
How much force a muscle can produce depends on two things: the contractile proteins themselves, and the connective tissues in the muscle and tendon that add force via elastic properties. This arrangement can be illustrated by the Hill muscle model [11].
Three-element Hill muscle model
(http://www.pt.ntu.edu.tw/hmchai/BM03/BMmaterial/Muscle.htm)
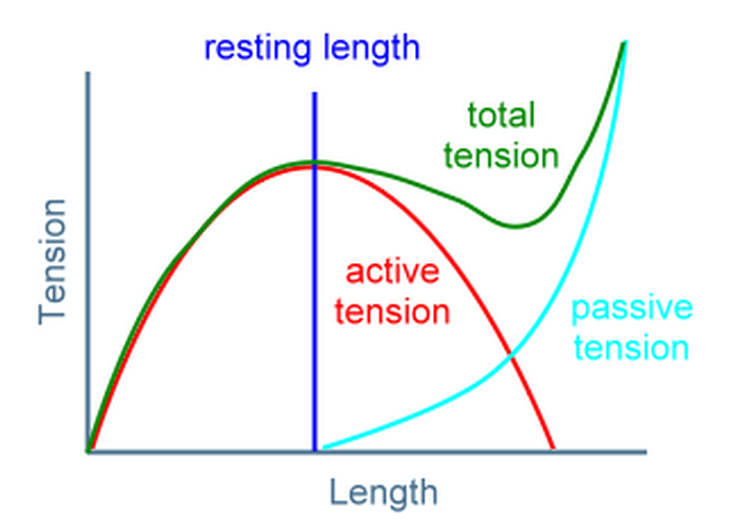
Both active and passive muscle force depend on the length of the muscle. Active force peaks when the muscle is around its resting length, and decreases when the muscle is shortened or lengthened. Passive force, on the other hand, works like a rubber band: It’s minimal when the muscle is shortened, and increases exponentially as the muscle lengthens [12].
Tissue Mechanics: Stress & Strain
In tissue mechanics, stress is a measure of the internal resistance a muscle develops in response to an applied load. Strain reflects the change in length caused by the imposed load. A muscle’s susceptibility to strain injury is determined by its mechanical response to loading. This response is modeled by a stress-strain curve. The slope of the curve represents the tissue’s stiffness, or tendency to resist length change. The area under the curve represents the strain energy stored by the tissue [10].
Strain energy is the key determinant of injury.
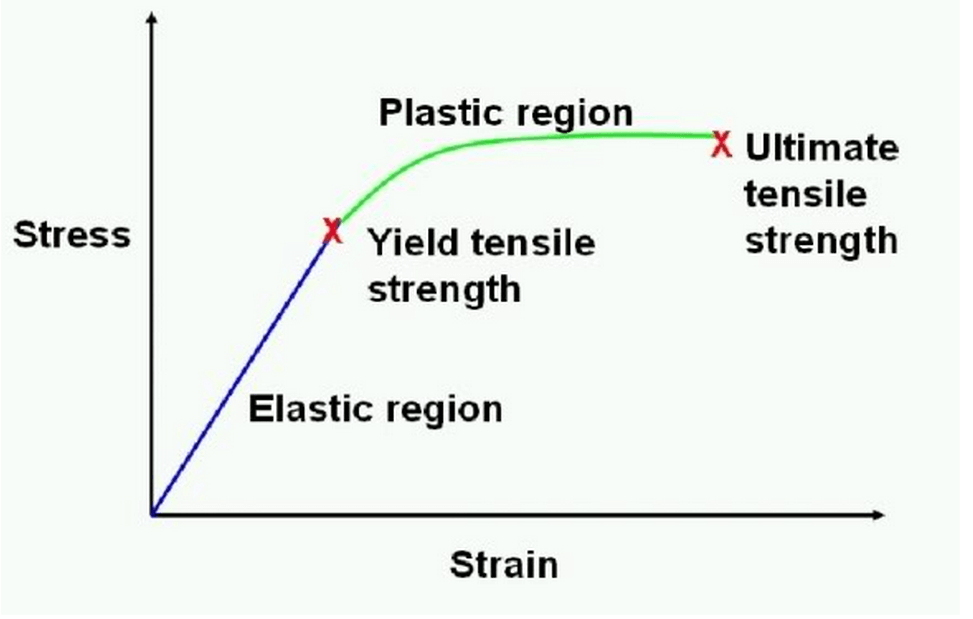
An idealized model of a passive (inactivated) muscle illustrates two predominant loading regions: the elastic region and the plastic region. In the elastic region, due largely to the elastic protein titin, passive muscle acts like a spring with a constant stiffness (the stress-strain curve maintains a constant slope). That is, it strains linearly with stress and returns to its original length without injury when the stress is removed [10]. At the extreme of the elastic region, just prior to the yield point, stress can reach up to 80% of its ultimate, failure-inducing value without injury [13].
Idealized stress-strain curve
(http://www.thumpertalk.com/topic/832301-quiz-time–-bolted-assemblies/page-5)
The stress-strain behavior of muscle begins to change as the load increases. When stress exceeds the yield point, muscle enters the plastic region. In this region, strain no longer increases linearly. Here, a small amount of additional stress results in a large strain. Unlike a rubber band, even when the stress is removed, the muscle does not return to its original length, but rather remains permanently deformed. Clinically, this deformation represents a partial muscle tear.
At the extreme end of the curve, where ultimate tensile strength is reached, the muscle can no longer withstand the stress and strain. At this point, mechanical failure – a complete tear of the muscle – occurs [10]. A muscle will completely tear at somewhere around 158% and 165% of its resting length [14].
A material’s mechanical response to loading depends on the characteristics of the material it’s made of. Muscle’s stress-strain behavior is due in part to its fluid composition, which makes it viscoelastic. That is, in conjunction with elasticity, muscle also has the property of viscosity, or resistance to motion (like molasses).
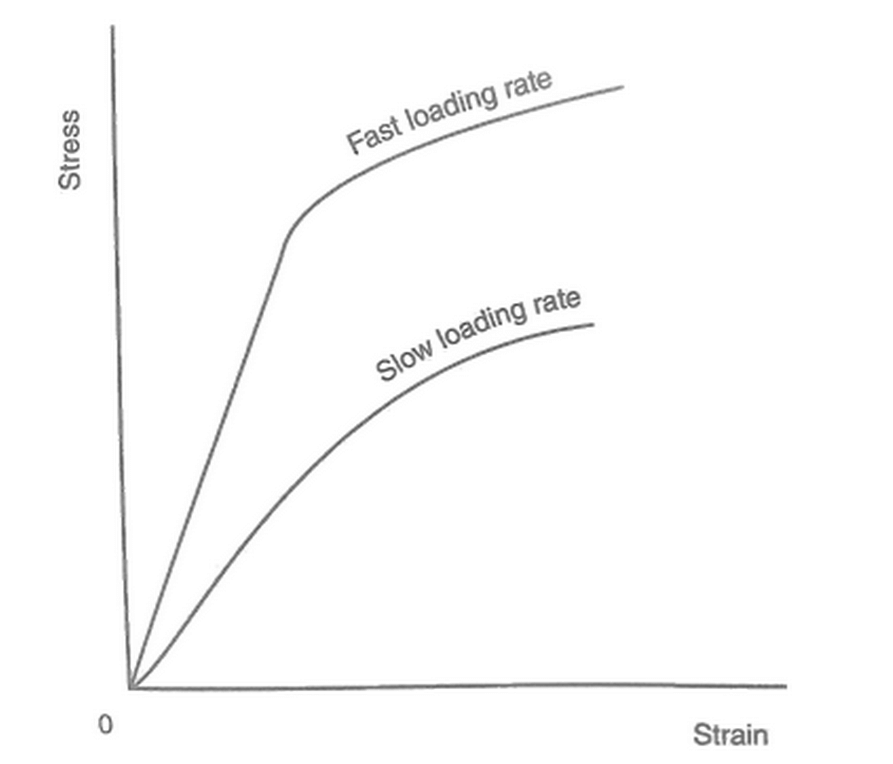
Viscoelasticity is responsible for muscle’s plasticity and also results in an important protective mechanism: strain-rate dependence. As the speed of application of loading increases, stiffness also increases, and the tissue is able to absorb more strain energy [10].
Strain-rate dependence [14]
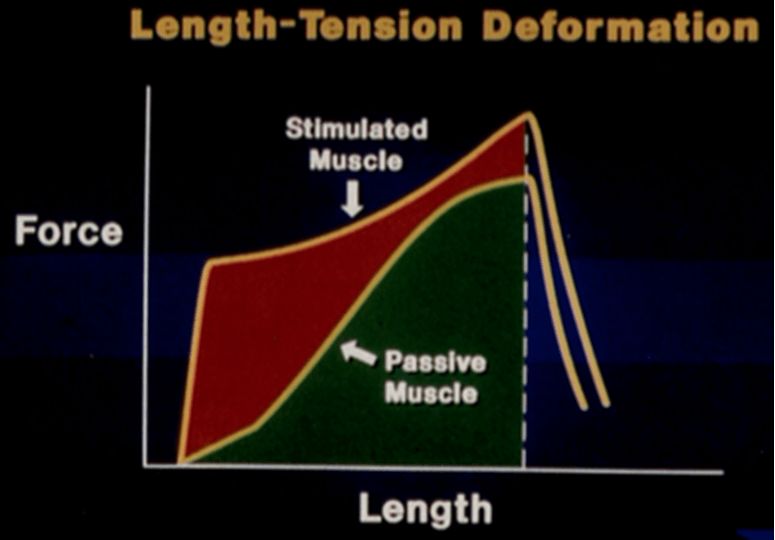
Of course, as discussed in the previous section, muscle is not simply a passive system. In fact, muscle is unique because it can be almost as compliant as skin when passive and almost as stiff as bone when contracting [10]. Thus, the true stress-strain behavior of muscle depends on the degree of muscle activation as well as time course of application of load, as per its strain-rate dependence.
Stress-strain curve for stimulated vs. passive muscle [15]
Two classic studies of animal muscles found increases in ultimate stress and strain energy at failure in stimulated muscle compared to non-stimulated muscle [15,16], likely due to increased cross-bridge formation [17]. No difference was observed in the ultimate strain (the amount of lengthening before failure) [10]. These findings suggest that regardless of activation, muscle will fail at the same ultimate length. However, it takes more energy to injure active muscle.
Stimulated isolated frog muscle
Mechanism, Signs, & Symptoms of Injury
Although the cause of acute muscle strains is often complex and multifactorial, most strains in strength training do share several common features. They generally occur:
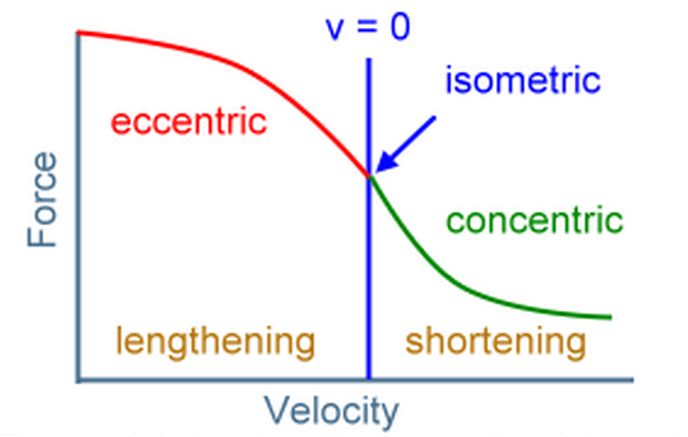
- During excessively high-load eccentric (lengthening) contractions, when muscles are capable of generating their highest active and passive forces. (The force of an eccentric contraction is often several times greater than maximal isometric force [18].)
- In biarticular muscles (two-joint muscles, like the biceps or hamstrings), which are subject to stretch at two joints [1].
- In muscles that contain predominantly fast-twitch (Type II) fibers [1].
Because strain injuries are a function of the total strain energy absorbed, they do not always occur at a muscle’s end range of motion [12].
Force-velocity curve of a muscle
(http://www.pt.ntu.edu.tw/hmchai/BM03/BMmaterial/Muscle.htm)
The precise location of a tear is a function of the distribution of stress throughout the tissue, but it’s most likely to happen near the junction between the muscle and tendon, because the transitional tissue is a bit weaker than either the muscle or tendon [10, 16].
The muscles most susceptible to strain injury include the hamstrings, quadriceps, hip adductors, hip flexors, abdominals, calves, and biceps [19]. Pec tears are on the rise as well, likely because men are increasingly getting in touch with their inner bench bro [1]. Unsurprisingly, pec major tears seem to occur almost exclusively in men [20].
Powerlifter Scot Mendelson with a torn pec
(http://fitnessorstrength.com/powerlifter/scot-mendelson-benchpress-injury/)
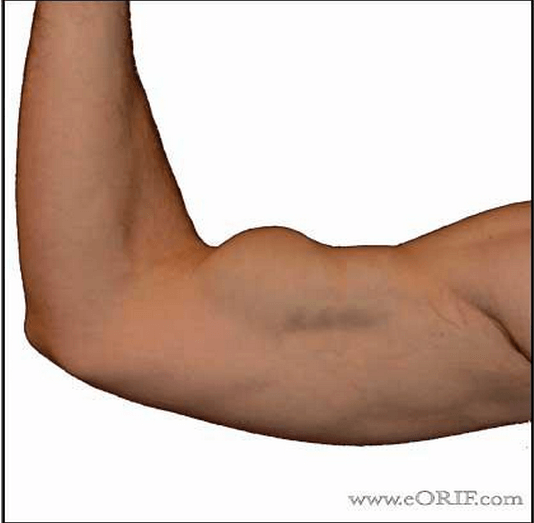
If you have a complete muscle tear, you’ll know it. A telltale sign of a complete tear is an audible pop, along with a tearing sensation. Generally, this is accompanied by immediate loss of function and intense pain, along with some pretty gnarly swelling and bruising that peak the day after the tear [19]. In the case of a complete tear, a pronounced “Popeye” deformity often happens as well.
“Popeye” bicep
(http://www.eorif.com/Elbowforearm/Images/Bicep-RuptureLH.jpg)
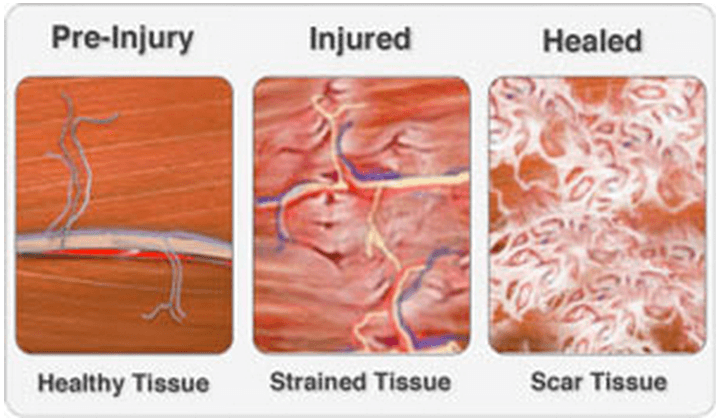
Once the inflammation goes down, scar tissue replaces injured muscle fibers. In the case of a mild partial tear, the scar is small, and surrounding muscle fibers can hypertrophy with no resulting functional deficit [19]. However, severe tears can result in the formation of dense, inelastic scar tissue that impairs muscle function to the point of contracture and chronic pain. Severe strains that prove resistant to conservative therapy often require surgical intervention. Training while injured or without proper rehabilitation can result in re-injury or increased severity of injury, as well as long-term recurrent muscle strains [1].
Formation of scar tissue following muscle strain
(http://properpillow.com/scar-tissue-fibrosis-chronic-pain/)
Predisposing Factors
There are several factors that predispose muscles to strain injury. The strongest predictor of injury is history of previous muscle injury [13]. Scar tissue is weaker and less elastic than the surrounding tissue, making it the weakest link in the musculotendinous unit and thus most susceptible to injury.
Fatigue, both of the muscle as well as the central nervous system, also plays an important role in strain injury. Continued loading of a fatiguing muscle will result in eventual mechanical failure, just like any other material [10]. With fatigue, elasticity of the muscle and tendon decrease, reducing the amount of strain energy they can absorb [17]. Fatigue of the central nervous system even further predisposes strength trainees to injury due to its interference with proper movement patterns [12].
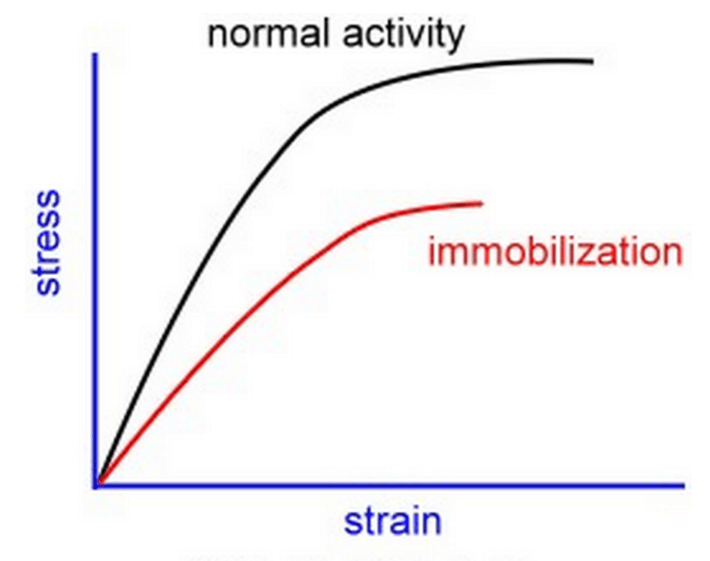
Other things that contribute to muscle strains include poor stability and muscle imbalance [1], as well as previous immobilization, weakness, cold temperatures [19], and unexpected cool-down [17]. All of these things tend to reduce muscle’s contractile capability and, consequently, its ability to absorb strain energy. Finally, it stands to reason that inflexibility would increase the risk of injury [21,22], although the evidence on this point is mixed and likely task-specific [23].
Effect of immobilization on muscle stress-strain behavior
(http://www.pt.ntu.edu.tw/hmchai/BM03/BMmaterial/Muscle.htm)
Because muscle strain injuries often occur at the musculotendinous junction, tendon strength is another key determinant of injury risk. The degeneration of a tendon’s collagen fibers occurs both with age [19] and systemic illness such as diabetes and rheumatoid arthritis [1]. The use of anabolic steroids has also been reported to cause tendon weakness, though not always [24,25]. It may be that steroid use increases muscle strength faster than the tendon can adapt, resulting in comparative weakness [26].
Injury Reduction Strategies
So, how do you reduce your risk of muscle strains? By fighting against all of the factors mentioned above that reduce the amount of strain energy a muscle can absorb!
So, what does that entail?
An adequate warm-up prior to training consisting of stretching and low-intensity aerobic activity can serve to increase range of motion, muscle temperature, and elasticity, which results in increased force production and strain energy absorption [17]. The ability of acute stretching for general injury prevention has largely been disproven. However, it has been shown to reduce the incidence of muscle strain injuries. To reduce the risk of stretching-related performance decrements, follow static stretching with dynamic stretching [27].
During your workout, you need to focus on lifting with proper technique (duh) [12,28]. You also need to be sure you’re doing enough warm-up sets prior to your work sets (duh) [29]. Other things that help include not going too crazy with loading or training volume, and resting long enough between sets (long enough that your breathing slows back down, but not long enough to get cold) [12, 18]. Potential gains in performance must always be weighed against the possibility of an interruption in training due to injury [30].
From a long-term standpoint, injury reduction strategies parallel many of the same basic tenets of general performance enhancement. These strategies include:
- Improved stability and task-specific flexibility [31].
- Conditioning to delay the onset of fatigue [1,17].
- Reduction in muscle imbalances (agonist-antagonist as well as side to side) [23].
- Progressive overload using hypertrophy [17], (eccentric) strength [1], and power [32] protocols for increased tensile strength of muscles and tendons.
- Proper periodization of all of the aforementioned training variables.
Eccentric hamstring training
(http://www.unchainedfitness.com/blog/eccentric-hamstring-training-the-emerging-paradigm-in-injury-prevention)
Future Directions
Over the last decade, strength sports have witnessed a surge in popularity. Despite medical advancements, the risk of injury remains the same as it has for decades [1]. Accordingly, understanding the mechanism of injury and reduction strategies are of the utmost importance, especially given the high likelihood of recurrence after the first incident.
The primary roadblock to progress may lie in the relative lack of good scientific evidence. The majority of the published literature focuses only on hamstring strains, and sample sizes are generally small. To help matters, a worldwide registration system for muscle injury would bolster the pool of evidence [1].
Unfortunately, direct measurement of the injury mechanism at the microscopic level is impossible at present. In an ideal world, researchers could study muscle strains in human subjects using three-dimensional movement analysis in a controlled laboratory setting. However, for some unknown reason, ethics boards are leery about approving studies where you purposefully tear people’s muscles. Fortunately, the latest wireless motion-capture technology, which uses high-speed, mobile sensors that can be applied directly to an athlete’s skin while in action, may soon make what was previously a scientific pipe dream a reality [1].
Wireless motion capture technology (http://www.biosynsystems.net/f-a-b-system)
• • •
Next: Benefits of Static Stretching Stretched out of Proportion? →
References
[1] Kerkhoffs G, Servien E, editors. Acute Muscle Injuries. Heidelberg, Germany: Springer; 2014.
[2] Winwood P, Hume P, Cronin J, Keogh J. Retrospective Injury Epidemiology of Strongman Athletes. J Strength Cond Res 2014;28:28–42.
[3] Siewe J, Marx G, Knöll P, Eysel P, Zarghooni K, Graf M, et al. Injuries and Overuse Syndromes in Competitive and Elite Bodybuilding. Int J Sports Med 2014;35:943–8.
[4] Calhoon G, Fry AC. Injury Rates and Profiles of Elite Competitive Weightlifters. J Athl Train 1999;34:232–8.
[5] Hak PT, Hodzovic E, Hickey B. The Nature and Prevalence of Injury During CrossFit Training. J Strength Cond Res 2013.
[6] Keogh J, Hume P, Pearson S. Retrospective Injury Epidimiology of One Hundred One Competitive Oceania Power Lifters: The Effects of Age, Body Mass, Competitive Standard, and Gender. J Strength Cond Res 2006;20:672–81.
[7] Zwingenberger S, Valladares RD, Walther A, Beck H, Stiehler M, Kirschner S, et al. An Epidemiological Investigation of Training and Injury Patterns in Triathletes. J Sports Sci 2014;32:583–90.
[8] Mendiguchia J, Alentorn-Geli E, Brughelli M. Hamstring strain injuries: are we heading in the right direction? Br J Sports Med 2012;46:81–5.
[9] Marieb E, Hoehn K. Human Anatomy & Physiology. 9th ed. San Francisco, CA: Benjamin Cummings/Pearson; 2013.
[10] Whiting W, Zernicke R. Biomechanics of Musculoskeletal Injury. 2nd ed. Champaign, IL: Human Kinetics; 2008.
[11] Winters JM. Hill-Based Muscle Models: A Systems Engineering Perspective. In: Winters J, Woo S, editors. Mult. Muscle Syst. Biomech. Mov. Organ., New York: Springer; 1990, p. 69–93.
[12] Stone M, Fry A, Ritchie M, Stoessel-Ross L, Marsit J. Injury Potential and Safety Aspects of Weightlifing Movements. Strengh Cond 1994;16:15–21.
[13] Garrett W. Muscle Strain Injuries: Clinical and Basic Aspects. Med Sci Sports Exerc 1990;22:436–43.
[14] McGinnis PM. Biomechanics of Sport and Exercise. 3rd ed. Champaign, IL: Human Kinetics; 2013.
[15] Garrett W, Safran M, Seaber A, Glisson R, BM R. Biomechanical Comparison of Stimulated and Nonstimulated Skeletal Muscle Pulled to Failure. Am J Sports Med 1987;15:448–54.
[16] Tidball J, Salem G, Zernicke R. Site and Mechanical Conditions for Failure of Skeletal Muscle in Experimental Strain Injuries. J Appl Physiol 1993;74:1280–6.
[17] Safran M, Seaber M, Garrett Jr. W. Warm-up and muscular injury prevention an update. Sport Med 1988;8:239–49.
[18] Enoka R. Neuromechanical Basis of Kinesiology. 2nd ed. Champaign, IL: Human Kinetics; 1994.
[19] Zarins B, Ciullo J. Acute Muscle and Tendon Injuries in Athletes. Clin Sports Med 1983;2:167–82.
[20] Aärimaa V, Rantanen J, Heikkilä J, Helttula I, Orava S. Rupture of the pectoralis major muscle. Am J Sports Med 2004;32:1256–62.
[21] Cross KM, Worrell TW. Effects of a Static Stretching Program on the Incidence of Lower Extremity Musculotendinous Strains. J Athl Train 1999;34:11–4.
[22] Haykowsky M, Warburton D, Quinney H. Pain and Injury Associated with Powerlifting Training in Visually Impaired Athletes. J Vis Impair Blind 1999;93:236–41.
[23] McHugh MP, Cosgrave CH. To stretch or not to stretch: the role of stretching in injury prevention and performance. Scand J Med Sci Sports 2010;20:169–81.
[24] Evans NA, Bowrey DJ, Newman GR. Ultrastructural Analysis of Ruptured Tendon From Anabolic Steroid Users. Injury 1998;29:769–73.
[25] Horn S, Gregory P, Guskiewicz KM. Self-reported Anabolic-androgenic Steroids Use and Musculoskeletal Injuries: Findings from the Center for the Study of Retired Athletes Health Survey of Retired NFL Players. Am J Phys Med Rehabil 2009;88:192–200.
[26] Petilon J, Carr DR, Sekiya JK, Unger D V. Pectoralis Major Muscle Injuries : Evaluation and Management. J Am Acad Orthop Surg 2005;13:59–68.
[27] Peck E, Chomko G, Gaz D V, Farrell AM. The effects of stretching on performance. Curr Sports Med Rep 2014;13:179–85.
[28] Haupt H. Upper Extremity Injuries Associated with Strength Training. Clin Sports Med 2001;20:481–90.
[29] Mazur L, Yetman R, Risser W. Weight-Training Injuries. Common Injuries and Preventative Methods. Sport Med 1993;16:57–63.
[30] Fisher J, Steele J, Brzycki M, DeSimone B. Primum non nocere: A commentary on avoidable injuries and safe resistance training techniques. J Trainology 2014;3:31–4.
[31] Linklater JM, Hamilton B, Ch MBB, Carmichael J, Orchard J, Ph D, et al. Hamstring Injuries : Anatomy, Imaging, and Intervention. Semin Musculoskelet Radiol 2010;1:131–61.
[32] Stone MH. Explosive Exercises and Training. Strength Cond J 1993;15:6–19.
[33] Monroy JA, Powers KL, Gilmore LA, Uyeno TA., Lindstedt SL, Nishikawa KC. What Is the Role of Titin in Active Muscle? Exerc Sport Sci Rev 2012;40:73–8.
[34] Hootman JM, Dick R, Agel J. Epidemiology of collegiate injuries for 15 sports: Summary and recommendations for injury prevention initiatives. J Athl Train 2007;42:311–9.